Delayed immune responses may drive COVID-19 mortality rates among men and the elderly
COVID-19 (SARS-CoV-2) infections tend to be more severe among older adults and males, yet the mechanisms underlying increased mortality in these two demographics are unknown. A study published in the open access journal PLOS Biology on September 8, 2020 by Nicole Lieberman and Alexander Greninger at University of Washington and colleagues suggests that varying immune responses to SARS-CoV-2 due to age and sex may depend on viral load and the time-course of infection
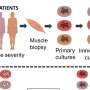
The clinical manifestations of COVID-19 vary widely across different patient populations, despite the virus's limited genetic diversity. To better understand the mechanisms that drive the diverse responses of infected individuals (hosts) among different patient demographics, researchers extracted and sequenced viral RNA from swabs collected from 430 COVID-19 positive cases and 54 negative controls. The scientists then analyzed the hosts' antiviral and immune responses across infection status, viral load, age and sex.
Researchers found that immune cell responses were not activated until after three days following the onset of infection, and that immune cell composition and function fluctuated with viral loads, in a way that suggested a dysfunctional antiviral response in males and the elderly. While these findings have important implications for development of immunomodulatory treatments for SARS-CoV-2, additional studies are needed as swabs were taken from the nasopharynx, which is not a sensitive anatomic location for accurately examining markers of systemic inflammation.
Elderly individuals as well as men have suffered higher mortality rates since the onset of the SARS-CoV-2 pandemic and may indicate weaker immune responses underlying poor clinical outcomes. According to the authors, "Collectively, our data demonstrate that host responses to SARS-CoV-2 are dependent on viral load and infection time with observed differences due to age and sex that may contribute to disease severity."
More information: Lieberman NAP, Peddu V, Xie H, Shrestha L, Huang M-L, Mears MC, et al. (2020) In vivo antiviral host transcriptional response to SARS-CoV-2 by viral load, sex, and age. PLoS Biol 18(9): e3000849. doi.org/10.1371/journal.pbio.3000849