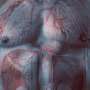
Results from COMBINE (OCT-FFR) reported at TCT Connect
Data from COMBINE (OCT-FFR) found that the use of FFR combined with OCT imaging can help improve the accuracy of high-risk lesion identification in patients with diabetes.
Findings were reported today at TCT Connect, the 32nd annual scientific symposium of the Cardiovascular Research Foundation (CRF). TCT is the world's premier educational meeting specializing in interventional cardiovascular medicine.
Fractional flow reserve (FFR) is widely used to guide the revascularization strategy in the catheterization lab. The FAME I and FAME II trials have shown that stable ischemic heart disease lesions with FFR >0.80 can be safely treated medically, while PCI of lesions with FFR<0.80 may benefit from revascularization.
However, recent evidence has shown that in some patient subgroups such as diabetes mellitus (DM) and/or acute coronary syndrome (ACS), lesions with FFR>0.80 can have worse outcomes than in patients without DM or ACS, most likely due to plaque instability or rapid progression of atherosclerotic plaque.
Previous studies have shown that lipid-rich plaques with a thin cap fibroatheroma (TCFA) have unfavorable clinical outcomes compared to non-TCFA lesions particularly in DM patients. Optical coherence tomography (OCT) can accurately identify lipid-rich and TCFA lesions. Whether OCT can identify lesions with future unfavorable clinical events despite lack of ischemia has not been studied previously.
The COMBINE (OCT-FFR) trial was a prospective international, natural history study. Patients with DM and with stable or acute coronary syndromes who had one or more non-culprit target lesion(s), with a 40-80% diameter stenosis, underwent FFR assessment. FFR-negative patients underwent OCT assessment and were further medically treated. Depending on the presence or absence of TCFA, patients were divided in two groups: TCFA negative (group A) and TCFA positive (group B). Patients with target lesions with FFR<0.80 were revascularized (group C).
The primary endpoint was the incidence of target lesion related MACE defined as cardiac death, target vessel myocardial infarction (MI), clinically-driven target lesion revascularization (TLR), or hospitalization due to unstable or progressive angina at 18 months in the medically treated patients with FFR>0.80 and TCFA patients (Group B) compared with medically treated patients with FFR>0.80 and no-TCFA (Group A). The secondary endpoint was the incidence of MACE between patients with FFR>0.80 and TCFA (Group B) vs. revascularized lesions that had FFR<0.80 (Group C).
The primary endpoint occurred in 13.3% of Group B compared with 3.1% of Group A [HR 4.7 95%CI (2.0-10.9) P=0.0004], suggesting that the presence of TCFA even in the absence of an abnormal FFR was predictive of future events. This rate of adverse events was even higher than the rate of events among the revascularized lesions with abnormal FFR at baseline (Group C) [HR 1.25 95%CI (0.28-5.59) P=0.77].
"In patients with diabetes, COMBINE (OCT-FFR) showed that the presence of a high-risk plaque (TCFA) is a strong predictor of future MACE, despite lack of ischemia," said Elvin Kedhi, MD, Ph.D. Dr. Kedhi is Professor of Cardiology, working in ULB (Liberal University Brussel) Hopital Erasme and Silesian Medical University, Katowice, Poland
"Additionally, patients with high-risk plaques (TCFAs) have a significant increase in target-lesion related MACE and MI compared to patients without TCFA at 18 months. These findings indicate that combining FFR and OCT can improve the accuracy of high-risk lesion and patient identification and should be adopted in practice."