Bio-based membranes with ocular stem cells to treat corneal disorders

The production, preparation, and use of bacterial nanocellulose as corneal bandages could be the key to help delicate stem cells to migrate to the cornea and heal the eye from a range of ocular disorders.
Our eyes have a very delicate surface that can be afflicted by a range of issues, like inflammatory diseases, burns, or acute trauma. The consequences of these ocular disorders (like opacification, vascularization, and scarring of the cornea) can cause a partial or total loss of vision.
A therapeutic answer can be found in limbal stem cells (LSC), which are located in the corneal limbus and replace lost cells in the cornea. A transplant of this type of cells into the affected area could heal the cornea, but that is a complex process because LSC are very delicate. To ensure efficient transplantation of cells, an appropriate substrate is required to affix the LSC to the cornea—a very specific combination of properties have to be achieved for a successful transplant.
Researchers from the Nanoparticles and Nanocomposites (NN) Group at the Institute of Materials Science of Barcelona (ICMAB, CSIC) have published an article on the production and characterization of bacterial nanocellulose (BNC) to be used as a bandage to secure LSC to the cornea. The study, published in Small, focuses on the use of LSC derived from human embryonic stem cells, and it was done in collaboration with the Eye Group lead by Prof. Heli Skottman in Tampere University (Finland), experts in the use of stem cells for ocular applications.
From bacteria to ex vivo testing
Irene Anton, researcher at the Nanoparticles and Nanocomposites (NN) Group, explains how the BNC is harvested, the first step of this process:
"Bacterial nanocellulose (BNC) is produced spontaneously as an extracellular polysaccharide by diverse types of bacteria. Almost the entire manufacturing process is done by the bacteria: we incubate liquid cultures of Komagataeibacter xylinus during 3-4 days, until a gelatinous hydrogel is formed at the interface between the liquid culture medium and the air. This film is then cleaned and sterilized and it can be used in our biomedical projects."
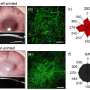
The LSC are attached to the nanocellulose with the help of an extracellular matrix coating, that is added previously to the bandages. A plasma reactor is used to achieve homogeneous and complete coating of the BNC. These samples are characterized through a series of experiments and techniques, such as measurements of light transmittance through the sample or studies on the viability of the cells. This study also includes preliminary ex vivo evaluation of the BNC on a Porcine Corneal Organ Culture as a simulated transplantation scenario.
"The ex vivo culture of pig eyes is a very convenient, cheap and ethical model to conduct preliminary studies of biomaterials addressed to the ocular surface. It allows evaluating simple but very relevant aspects of the materials such as: can it be sutured to the ocular surface? Is it robust enough to be placed in the cornea for a certain amount of time? Is it easy to manipulate? The size of the pig eyes is quite similar to those of humans and regeneration of the corneal epithelium can be studied because the cells of the cornea are alive during the culture. The limitation is that there is no intervention of the immune system and therefore we cannot conclude if BNC will cause immune reactions or not. For that, we would need the whole animal."
Advantages of using bacterial nanocellulose as ocular bandage
Bacterial nanocellulose is just one of the many options being studied for this application. Other natural polymers, such as collagen, fibrin, or hyaluronic acid are quite popular. Even synthetic substrates made by electrospinning seem promising.
However, BNC has many properties that make it a good candidate for ocular surface bandaging: "BNC has some advantages such as its thermal stability, which allows not only sterilization at high temperature, but also cryopreservation in nitrogen tanks. Besides, as mentioned before, the production process is quite simple and there is no need to use hazardous chemicals or to do any synthesis step. Another advantage of BNC is that it can be shaped to any format and functionalized by many different routes."
Moreover, the study has shown that BNC allows human LSC to create new daughter cells and to survive for quite long periods while keeping their stem cells characteristics. At the same time, it provides a self-standing and easy to manipulate mechanical support.
This tissue has many advantages thanks to its biocompatibility, robustness and conformability to the domed shape of the cornea. However, one key factor hinders its potential use, and it is the fact that BCN is not fully transparent. "Therefore, for now, we cannot think about artificial corneas made of BNC. Rather, we are focusing on temporal bandages used to treat a corneal pathology during a certain amount of time and then removed when the pathology has improved."
The future of bacterial nanocellulose as cell carrier
This study represents progress for this biotechnology product, but Irene Anton already has her eyes in the future, where BNC could even be used as cell carrier in other therapeutic treatments: "My long-term vision is to provide ready-to-use therapeutic products consisting of LSC seeded on top of BNC membranes that are easy to use and available to as many hospitals as possible. For that, we need a storage method, probably cryostorage, and of course to scale up the production of both cells and BNC and to meet all the regulatory requirements. There is still a lot of work to do."
More information: Irene Anton‐Sales et al. Limbal Stem Cells on Bacterial Nanocellulose Carriers for Ocular Surface Regeneration, Small (2021). DOI: 10.1002/smll.202003937