Building equity into vaccine distribution

As the U.S. speeds up distribution of COVID-19 vaccines, the question of equity keeps surfacing. Who gets priority? If the pandemic is hitting certain communities harder, can they be adequately supplied with vaccine doses? What's the best way to balance the needs of different groups within society?
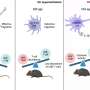
MIT economist Parag Pathak's work emphasizes those questions—and helps tackle them. Over the last year, Pathak and a group of colleagues have developed an approach to the distribution of vaccines and other medical goods that is being used in Massachusetts, New Hampshire, and Tennessee.
This approach, called either a "reserve system" or a "categorized priority system," allows medical resources to be allocated among multiple groups at once, while retaining enough flexibility to help groups with especially acute needs. In practice, a vaccine can be distributed among frontline medical workers and senior citizens while also reaching places that have been especially hard-hit by COVID-19.
"The reserve system offers a way to get to some compromise, where you still respect the prioritization of frontline workers and the elderly, but you also have a way to scale up to how you want to protect the most disadvantaged communities," says Pathak, the Class of 1922 Professor of Economics.
That need certainly exists: Geographically, the pandemic has taken a heavy toll in many hotspot areas across the country. Demographically, as a Jan. 26 CNN analysis of 14 states showed, about 4% of the white Americans have been vaccinated so far, compared to just 1.9% of Blacks and 1.8% of Hispanics.
From ventilators to vaccines
Since early 2020, Pathak has been working on these resource-allocation issues with a group of colleagues—especially Boston College economics professors Tayfun Sönmez and Utku Ünver, who like Pathak specialize in designing markets for nonfinancial goods, and University of Pennsylvania medical ethicist Harald Schmidt. Last spring, they proposed a way for states to allocate ventilators across multiple groups in society.
The group realized the reserve system could be extended to COVID-19 therapeutics and vaccines. Since then, they have produced multiple working papers analyzing vaccine distribution and the reserve system; developed a modeling tool for health officials; and met with policymakers from across the country. They also hosted an online conference on vaccine allocation and social justice in December with Ariadne Labs at Harvard University and the Leonard Davis Institute at the University of Pennsylvania, with over 500 participants.
Massachusetts has now adopted reserve system principles for the distribution of both COVID-19 vaccines and the monoclonal antibody treatment, while Tennessee is using the reserve system for vaccines as well.
"Massachusetts and Tennessee have embraced this concept," Pathak says. "These are very concrete steps toward equitable vaccine distribution."
Over the last year, Pathak and his colleagues have produced "sophisticated mathematical models that were simply unknown within the world of medicine and public health," says Robert Truog, director of the Harvard Center for Bioethics, Frances Glessner Lee Professor of Legal Medicine, and professor of anesthesia at Harvard Medical School. "The approaches that they are developing go a long way toward addressing difficult concerns about social justice within complex problems such as the fair allocation of COVID-19 vaccines." After encountering the group's work, Truog collaborated with them on a paper surveying the subject.
So what is the reserve system, exactly?
In the first place, the method distributes medical resources to multiple groups simultaneously, rather than ranking everyone on one priority scale. For COVID-19, Pathak and his colleagues recommend setting aside a portion of available vaccines for particularly hard-hit social groups.
In this way, "an ideal allocation mechanism should permit a wide range of options," as Sönmez, Pathak, Ünver, and their co-authors wrote in a paper recently published in CHEST, the journal of the American College of Chest Physicians.
In Tennessee, 85% of vaccine doses are distributed across the state; 10% go to disadvantaged areas, as measured by the Social Vulnerability Index of the Centers for Disease Control; and 5% are applied to hotspots that flare up. At least 27 counties have been allocated additional vaccine doses based on vulnerability to COVID-19. Massachusetts' plan recommends setting aside 20% of vaccines to communities that have a disproportionate COVID-19 burden and high social vulnerability.
To distribute monoclonal antibodies, Massachusetts also adopted a reserve system along the lines the scholars recommended, with 80% of the available doses allotted to a general category with various subdivisions, and another 20% of doses being for patients from disadvantaged areas.
This approach addresses a clear problem the economists have quantified: If vaccine distribution is proportional to population, it will lack the maximum impact in saving lives and preventing illness, because not all areas are equally affected.
The scholars modeled this in detail in a working paper posted last November, which looks at vaccine distribution nationally.
The result? A strictly population-based allotment means worse-off groups in 16 states—including California, Florida, New York, and Texas—would receive relatively fewer vaccine doses, compared to a system in which the federal government used 10% of doses for especially vulnerable groups nationwide.
In another recent working paper by the same authors, the researchers found that doubling the allotment for hard-hit groups to 20% more than doubles the number of particularly vulnerable people who would get vaccinated within the first 48 million doses.
"If you take into account the national distribution of who is hard hit, then you could do a lot more to advance the cause of equity," Pathak says. (The Biden administration has announced new federal support for more vaccination locations for disadvantaged communities.)
Not just a 10% solution
There is no magic reserve number—10% or otherwise— for disadvantaged populations. Instead, the group's work suggests a general principle: If there are greater social inequities, the quantity in a reserve allotment could rise. By contrast, if everyone were in the same medical circumstances, a priority system would be unnecessary.
"If it [the social landscape] were completely even, you wouldn't need a reserve," Pathak says.
There are other factors to weigh as well—such as whether Black or Hispanic populations are more reluctant to get vaccinated than the population in general.
"If you want to ensure equity, you have to keep track of the [vaccine] takeup as it progresses," Pathak says. "If there are very stark differences across demographic groups on vaccine takeup, and if our goal is not offers of vaccines, but actual vaccination, [a given percentage allotment] for the hardest-hit may not be adequate." If so, health officials might increase their reserve allotment for the truly disadvantaged.
"This all may sound like an arcane implementation issue, but really, that's what we're about," Pathak says. "I've always found it very valuable to interact with policymakers on the ground solving real problems, and to learn from them. With COVID, it's not about seeing whether we can find the optimal theoretical system, but seeing if we can engineer things to be just a little bit better."
More information: Tayfun Sönmez et al. Categorized Priority Systems, Chest (2020). DOI: 10.1016/j.chest.2020.12.019
Harald Schmidt et al. Rationing Safe and Effective COVID-19 Vaccines: Allocating to States Proportionate to Population May Undermine Commitments to Mitigating Health Disparities, SSRN Electronic Journal (2020). DOI: 10.2139/ssrn.3729069
Harald Schmidt et al. What Prioritizing Worse-Off Minority Groups for COVID-19 Vaccines Means Quantitatively: Practical, Legal and Ethical Implications, SSRN Electronic Journal (2020). DOI: 10.2139/ssrn.3716686
This story is republished courtesy of MIT News (web.mit.edu/newsoffice/), a popular site that covers news about MIT research, innovation and teaching.