Modeling COVID-19 infection based on movement can improve public health response
An epidemic like COVID-19 relies on infected people mixing with uninfected people—encounters that typically require one or both to move around. A new method for modeling the progression of pandemic infections incorporates location data from smartphones to give public health policymakers a more accurate picture of the way people in their communities are mixing and where and how to focus their efforts.
"Most models of COVID-19 take a county or a group of census tracts and treat the population in many ways as a homogenous group," says Song Gao, geography professor and member of the group of University of Wisconsin–Madison researchers who described the new modeling method this week in the Proceedings of the National Academies of Sciences. "When we looked at reports on census tracts, we saw some with a high infection rate, but neighboring tracts with low confirmed cases."
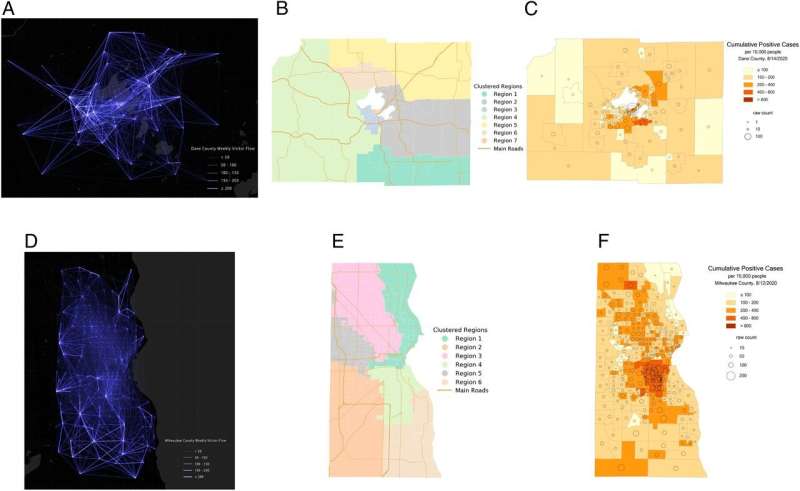
That made mixing between residents of the neighboring tracts seem unlikely, so the researchers gave anonymized data on the trip origins and destinations of cellular phones in Wisconsin's two most populous counties, Dane and Milwaukee, over to a machine learning algorithm that broke the counties down into new subregions.
"The algorithm uses the information on human mobility flow to repartition each county into smaller subregions in which there is high internal mobility. The people within each new subregion have the most interactions with each other," Gao says.
The researchers' new subregions revealed demographic separations that could be seen as key to the way COVID-19 infections peaked in each county.
"Dane County's most significant heterogeneity is the difference in age structure among neighborhoods," Gao says. "In Milwaukee County, the most significant difference is racial and ethnic diversity."
That squares with the way the counties experienced outbreaks in the summer of 2020. Dane County struggled with a spike in the infection rate in its youngest subregion, driven by clusters of infection centered on bars typically frequented by younger crowds. Milwaukee County's pandemic had an outsized effect on Black and Hispanic communities concentrated in two areas also identified via mobility data as relatively insular subregions.
"Modeling that accounts for mobility within and between these subregions gives us a better understanding of how the infection situation we are in happened, the opportunity to investigate some of what you might call super-spreading events, and can help policymakers investigate why a specific day has a very high rate of infection," says Gao, whose work is funded by the National Science Foundation.
The research team—which includes geographers, mathematicians, an epidemiologist and communications experts—used the model to examine decisions to ease restrictions in each county as the pandemic seemed to wane in mid-2020.
In steps in May and June, for example, Dane County allowed business (including bars) to open to 25 percent and then 50 percent their normal capacity on June 15. By June 30, in the markedly young subregion adjacent to UW–Madison, the infection rate rose to 11.6 cases per thousand residents. According to the mobility-inclusive method of mathematical modeling (not controlled experiments), not relaxing these checks on interaction would have limited the infection rate to 3.4 per thousand people—one-third the actual spread.
Incorporating mobility and foot traffic data can help public health agencies identify unique aspects of their communities that need to be addressed to arrest the spread of a pandemic virus.
"Instead of implementing one-size-fits-all policy, we can design policies that are region-specific, based on different types of heterogeneity," Gao says.
More information: Xiao Hou et al, Intracounty modeling of COVID-19 infection with human mobility: Assessing spatial heterogeneity with business traffic, age, and race, Proceedings of the National Academy of Sciences (2021). DOI: 10.1073/pnas.2020524118





















