Study shows rapid decrease in American lung cancer and melanoma deaths
Overall cancer death rates continue to decline in men and women for all racial and ethnic groups in the United States, according to the latest Annual Report to the Nation on the Status of Cancer. During 2001 to 2018, declines in lung cancer death rates accelerated, and death rates for melanoma declined considerably in more recent years, reflecting a substantial increase in survival for metastatic melanoma. However, the report finds that for several other major cancers, including prostate, colorectal and female breast cancers, previous declining trends in death rates slowed or disappeared.
The report, appearing in JNCI: The Journal of the National Cancer Institute, also finds that overall cancer incidence rates continue to increase among females, children, and adolescents and young adults (AYA). All trends in this report cover the period before the COVID-19 pandemic.
The annual report is a collaborative effort among the American Cancer Society (ACS); the Centers for Disease Control and Prevention (CDC); the National Cancer Institute (NCI), part of the National Institutes of Health (NIH); and the North American Association of Central Cancer Registries (NAACCR).
The report shows a decrease in death rates for 11 of the 19 most common cancers among men, and for 14 of the 20 most common cancers among women, over the most recent period (2014-2018). Although declining trends in death rates accelerated for lung cancer and melanoma over this period, previous declining trends for colorectal and female breast cancer death rates slowed and those for prostate cancer leveled off. Death rates increased for a few cancers like brain and other nervous system and pancreas in both sexes, oral cavity and pharynx in males, and liver and uterus in females.
"The declines in lung cancer and melanoma death rates are the result of progress across the entire cancer continuum—from reduced smoking rates to prevent cancer to discoveries such as targeted drug therapies and immune checkpoint inhibitors," said Karen E. Knudsen, MBA, Ph.D., Chief Executive Officer, American Cancer Society. "While we celebrate the progress, we must remain committed to research, patient support, and advocacy to make even greater progress to improve the lives of cancer patients and their families."
An analysis of long-term trends in cancer death rates in this year's report also shows that death rate declines accelerated in both males and females from 2001 to 2018. In males, a decline of 1.8% per year in 2001 to 2015 accelerated to a decline of 2.3% per year during 2015 to 2018. In females, a decline of 1.4% per year from 2001 to 2015 accelerated to a decline of 2.1% per year during 2015 to 2018. The report found that overall cancer death rates decreased in every racial and ethnic group during 2014 to 2018.
"It is encouraging to see a continued decline in death rates for many of the common cancers," said Karen Hacker, MD, MPH, Director of CDC's National Center for Chronic Disease Prevention and Health Promotion. "To dismantle existing health disparities and give everyone the opportunity to be as healthy as possible, we must continue to find innovative ways to reach people across the cancer care continuum—from screening and early detection to treatment and support for survivors."
However, increases in cancer incidence and death rates or deceleration of previous declining trends for some other cancers such as colorectal and female breast cancers are likely due to risk factors such as obesity.
"The continued decline in cancer death rates should be gratifying to the cancer research community, as evidence that scientific advances over several decades are making a real difference in outcomes at the population level," said Norman E. "Ned" Sharpless, MD, Director of the National Cancer Institute, of the National Institutes of Health. "I believe we could achieve even further improvements if we address obesity, which has the potential to overtake tobacco use to become the leading modifiable factor associated with cancer."
The authors report that cancer death rates continued to decrease among children (aged <15 years) and AYAs (aged 15-39 years) despite an increase in incidence rates from 2001 to 2017. Overall cancer incidence rates in children and AYA increased in all racial/ethnic groups except American Indian/Alaska Native (AI/AN) children where rates remained stable. The most common cancer among AYA was female breast cancer.
"When evaluating health disparities, it is critical to acknowledge the social factors that influence the health of the communities and access to health care," said Betsy A. Kohler, MPH, NAACCR Executive Director. "Social and economic indicators, particularly based on small area assessments, are increasingly important to understanding the burden of cancer."
Other key findings include:
- Overall cancer incidence rates were higher among men than women in every racial and ethnic group, except Asian/Pacific Islander population, where the rates were similar.
- Overall cancer incidence rates were slightly lower among Black people than White people.
- In contrast, overall cancer death rates were higher among Black people than White people.
- Incidence rates of liver cancer were previously increasing, but data show rates have stabilized among both men and women.
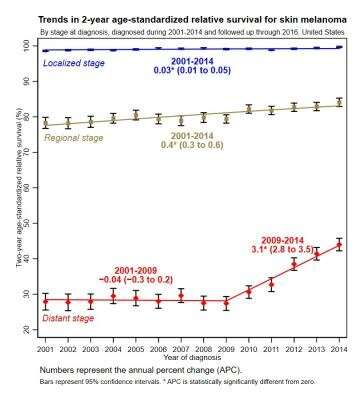
- Two-year relative survival for advanced-stage melanoma cases diagnosed during 2001-2009 was stable, but it increased 3.1% per year for those diagnosed during 2009-2014.
- Two-year relative survival only slightly increased for early- and intermediate-stage melanoma cases diagnosed during 2001-2014 (0.03% and 0.4% per year, respectively).
The authors indicate these findings can help inform healthcare providers about the need to increase efforts related to cancer prevention, early detection, and treatment, and for the need for equitable implementation of effective interventions, especially among under-resourced populations.
More information: Farhad Islami et al, Annual Report to the Nation on the Status of Cancer, Part I: National Cancer Statistics, Journal of the National Cancer Institute (2021). DOI: 10.1093/jnci/djab131