SARS-CoV-2 variant B.1.617 attacks immune system
SARS-CoV-2 still poses major challenges to mankind. The frequent emergence of mutant forms makes the threat posed by the virus difficult to predict. The SARS-CoV-2 variant B.1.617 circulated in India and gave rise to the Delta variant, B.1.617.2, which is now becoming dominant in many countries. Infection researchers from the German Primate Center (DPZ) – Leibniz Institute for Primate Research in Göttingen have investigated the B.1.617 variant in detail. In cell culture studies, they found that this variant can infect certain lung and intestinal cell lines more efficiently than the original virus. The researchers also demonstrated that B.1.617 is less sensitive to inhibition by antibodies present in the blood of convalescent or vaccinated individuals and resistant to a therapeutic antibody used for COVID-19 treatment. These properties may enable B.1.617 and its subtypes to rapidly spread in the human population, thereby increasing the risk of incompletely vaccinated individuals and individuals with declining immune protection to become infected (Cell Reports).
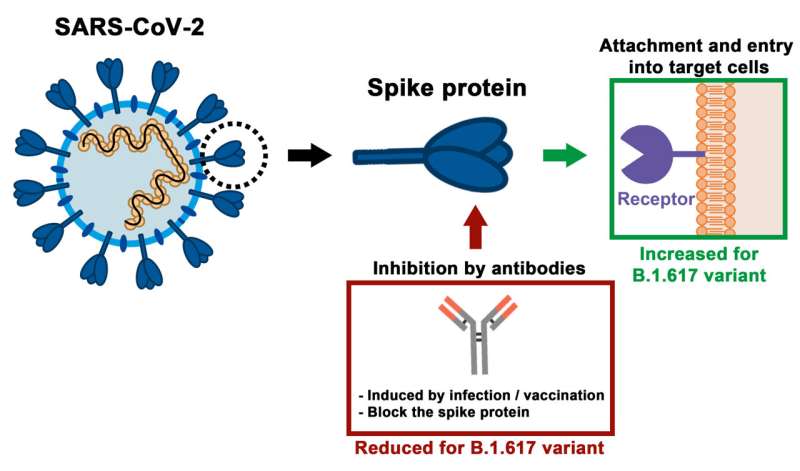
The spike protein is embedded in the viral envelope and facilitates SARS-CoV-2 entry into host cells. Without the activity of the spike protein the virus cannot replicate in the human body. The currently known virus variants harbor different mutations in the spike protein, some of which make it easier for them to infect host cells and evade the immune system of infected individuals. The B.1.617 variant carries eight different mutations in the spike protein, including two within the receptor binding domain, which is essential for viral attachment to cells and represents the main target for neutralizing antibodies.
A team led by Markus Hoffmann and Stefan Pöhlmann, infection researchers at the German Primate Center, and including scientists from the University Hospital of Göttingen, the University of Erlangen and the Hannover Medical School, investigated how the mutations impact the ability of the B.1.617 variant to enter host cells and how efficiently the antibody response in vaccinated and recovered individuals inhibits this variant.
First, the researchers analyzed entry of the B.1.617 variant into different human cell lines. In two cell lines derived from lung and colon, respectively, they detected a 50 percent increase in the virus' entry efficiency.
The researchers also investigated the efficacy of four different therapeutic antibodies that have been approved for the treatment of COVID-19 patients. They found that the B.1.617 variant was completely resistant against one of these antibodies and slightly less inhibited by another antibody.
In a third step, the scientists tested the efficacy of antibodies from the blood of recovered and vaccinated individuals. Here, they found a two- to threefold reduction in protection against the B.1.617 variant.
"Our study shows that this virus variant can infect lung and intestinal cells more efficiently, suggesting increased viral fitness," Markus Hoffmann, lead author of the study, summarizes the results. "In addition, the protective effect of antibodies is limited because they block the cell entry of B.1.617 less efficiently than that of the original virus. As a result, individuals who are not fully vaccinated or were infected a long time ago and thus produce low amounts of antibodies, may be poorly protected against infection with the B.1.617 variant.
Stefan Pöhlmann, Head of the Infection Biology Unit at the DPZ adds: "In order to prevent further spread of the B.1.617 variant, especially its subtype Delta, and to prevent the emergence of new virus variants it is advisable to quickly achieve full immunization of all people that are willing to be vaccinated. It is also necessary to investigate whether booster vaccinations with existing vaccines or vaccines optimized to target variants provide long-lasting and broad protection."
More information: Markus Hoffmann et al, SARS-CoV-2 variant B.1.617 is resistant to bamlanivimab and evades antibodies induced by infection and vaccination, Cell Reports (2021). DOI: 10.1016/j.celrep.2021.109415