Existing drug may help improve responses to cellular therapies in advanced leukemias
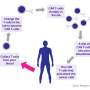
Too many "exhausted" T cells left in the wake of aggressive chemotherapy regimens for patients with advanced chronic lymphocytic leukemia (CLL) make it more challenging for chimeric antigen receptor (CAR) T cell therapy to do its job. Now, a new study from researchers in the Perelman School of Medicine at the University of Pennsylvania shows how to overcome this type of resistance and reinvigorate these T cells with an experimental small molecule inhibitor.
Reporting online today in the Journal of Clinical Investigation, the team shows how the drug, known as JQ1, improved CAR T cell function by inhibiting what is known as the bromodomain and extra terminal (BET) proteins. BET, the researchers showed, can disrupt CAR expression and key acetylated histone functions in T cells in CLL.
The findings demonstrate, for the first time, this mechanism of resistance and present a much-needed target for CLL when treating patients with cellular therapies like CAR. Only a small subset of patients with advanced CLL respond to CAR T cell therapy—compared to 80 percent of acute lymphocytic leukemia patients with advanced disease.
"Why CAR T cells fail to fully attack cancer cells in so many CLL patients is an important question that needs to be answered in order to expand the use of these immunotherapies in CLL and other cancers," said senior author Joseph A. Fraietta, Ph.D., an assistant professor of Microbiology at Penn, and member of the Center for Cellular Immunotherapies. "Treating these 'war weary' T cells during the CAR T cell engineering process has the potential to boost responses, we've shown here. It's setting the stage for a very promising set of next steps that rationalize further studies, including clinical trials, to prove this approach is safe and feasible."
Using the small molecule inhibitor and the T cells and CD19 CAR T cells from multiple previously treated patients, the researchers demonstrated that the BET protein plays a role in downregulating CAR expression, and that if blocked, can diminish CAR cell T cell exhaustion and increase the production of CAR T cells from CLL patients with poor lymphocytes.
Treatment with JQ1 also increased levels of various immunoregulatory cytokines and chemokines previously reported to be produced by CAR T cells in CLL during successful therapy. The array of native immune and CAR cells mirrored those found more typically in patients who do respond.
Given this observed reinvigoration of dysfunctional CLL patient CAR T cells by BET inhibition, the authors suggest that incorporating JQ1 into cellular engineering and expansion processes could lead to a generation of less defective and more potent final CAR T cells for patients.
To what extent the above pathways contribute to the effects of JQ1 on CAR T cells is a focus of ongoing investigations for the research group.
"This work shows us that T cells can be taught new tricks," said Bruce Levine, Ph.D., the Barbara and Edward Netter Professor in Cancer Gene Therapy in Penn's Perelman School of Medicine, and co-author on the study. "That is to say that the methods of manufacturing can be adapted to improve CAR T cell function, so that what would have been exhausted or dysfunctional cells can now be reinvigorated, and potentially lead to better clinical responses in more patients than before."