iPS cells show therapeutic benefits for a rare muscle dystrophy
Muscular dystrophy describes a family of congenital diseases that cause the progressive loss of muscle tissue. Severity varies across the family, but for many there is little in the way of treatment. In its newest study, which can be seen in Stem Cell Research & Therapy, the Hidetoshi Sakurai lab shows the benefits of iPS cell-based therapy for treating Ullrich congenital muscular dystrophy (UCMD) in mice. The transplanted cells secreted collagen VI, which stimulated the regeneration of lost muscle tissue.
UCMD is a rare progressive disease in which muscles atrophy. Patients show symptoms early in life and can rarely walk unassisted by puberty. No curative drugs exist, and patients are mainly managed through rehabilitation.
"All UCMD cases are due to a mutation in the COL6A1-3 genes. We are researching collagen VI supplementation by cell therapy as a treatment," explains Dr. Nana Takenaka-Ninagawa, a physiotherapist and one of the lead authors of the study. COL6A1-3 codes for collagen VI, an essential molecule for skeletal muscle stability.
The transplantation of mesenchymal stromal cells has already been shown to have therapeutic benefits on muscle cells in mouse models of UCMD. In fact, mesenchymal stromal cells are known to have therapeutic effects for all sorts of ailments, at least over a short period.
"It is not clear if the benefits are due to collagen VI supplementation or how long the effects last," said Takenaka-Ninagawa.
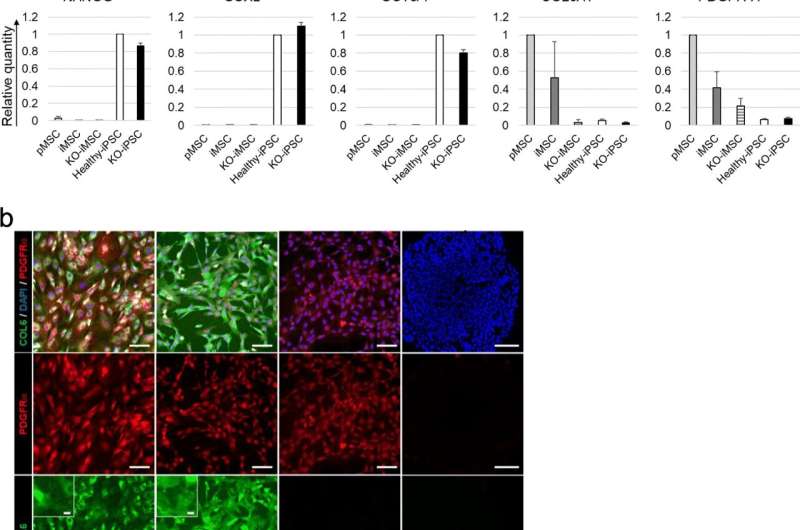
Therefore, she and colleagues prepared a selection of mesenchymal stromal cells made from iPS cells. These included those with normal COL6A1-3 genes, those with COL6A1 gene knocked out, and those made from UCMD patients who had a mutation in COL6A1 gene and thus could not produce healthy levels of collagen VI. These cells were then injected into mice with UCMD symptoms.
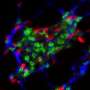
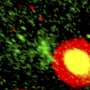
The study found only mice that received mesenchymal stromal cells with intact COL6A1-3 genes showed muscles with higher collagen VI levels, less UCMD symptoms, and more muscle regeneration. In contrast, none of these observations were made when mesenchymal stromal cells with defective COL6A1 gene were transplanted.
"We found a clear correlation between collagen VI supplementation and muscle regeneration," said Takenaka-Ninagawa.
The regeneration was attributed to the activation of muscle stem cells, which scientists had previously found was facilitated by collagen VI.
"Others have shown evidence that collagen VI supplementation by cell transplantation has therapeutic benefits on UCMD. But we did a long-term observation [24 weeks] and confirmed that the effects are sustained," said Sakurai.
More information: Nana Takenaka-Ninagawa et al, Collagen-VI supplementation by cell transplantation improves muscle regeneration in Ullrich congenital muscular dystrophy model mice, Stem Cell Research & Therapy (2021). DOI: 10.1186/s13287-021-02514-3