Simple donor-specific biomarker predicts liver transplant rejection independent of recipient
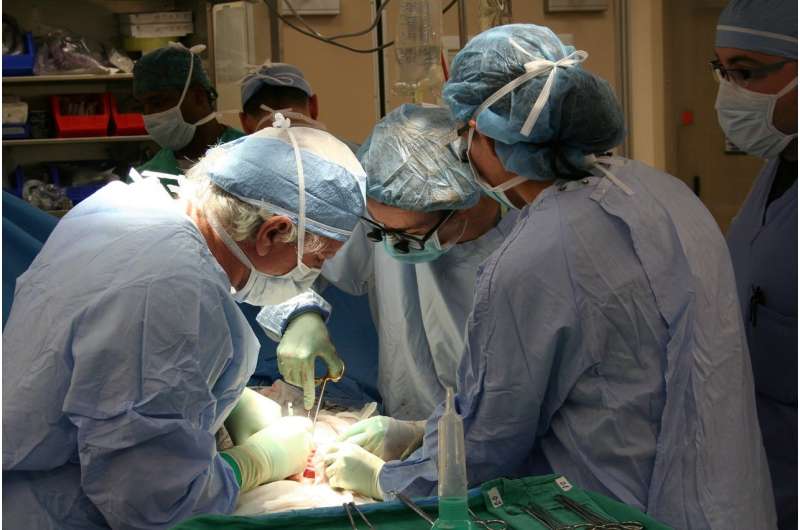
A cohort study found that class I HLA evolutionary divergence (HED) of the donor predicts acute or chronic rejection of a liver transplant. This prognostic marker can be found rapidly at no additional cost and has the potential to orientate donor selection and guide immunosuppression following transplantation. The findings are published in Annals of Internal Medicine.
Organ rejection depends on HLA proteins expressed by donor's and recipient's cells which are variable between individuals and thus are different between donors and recipients. Compatibility means that the more the HLA proteins are similar between donor and recipient, the less likely the organ is to be rejected. The HED, a continuous metric quantifying the peptidic differences between 2 homologous HLA alleles, reflects the breadth of the immunopeptidome presented to or by the immune cells.
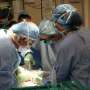
Researchers from the Assistance Publique, Hôpitaux de Paris, (France) studied health records for 1,154 adults and 113 children who had a liver transplant between 2004 and 2018 to assess the potential effect of donor or recipient HED on liver transplant rejection. They found that HED calculated from the HLA alleles of the donor, had a much stronger influence on liver transplant success than HLA compatibility. The higher the HED of a donor of liver graft, the more frequent rejection and this was completely independent of the HLA compatibility of donors and recipients. These findings suggest for the first time that a donor-dependent biomarker (independent of the recipient) can predict allograft rejection. This finding has significant implications in clinical practice.
More information: Annals of Internal Medicine (2021). https://www.acpjournals.org/doi/10.7326/M20-7957