Sharing vaccines is in countries' best interests

How nations can best allocate COVID-19 vaccines remains a discussion of global importance. And at its heart is the question of whether countries with greater access to vaccines should focus on vaccinating their own citizens or sharing their vaccine allotments with other nations.
While some argue that these high-income countries can reduce the overall number of global COVID-19-related deaths if they share the vaccine, a new Yale study finds it's in their interest, too.
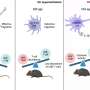
Writing in the journal Scientific Reports, the interdisciplinary and multi-institutional research team reports that once a country reaches herd immunity, sharing vaccines is better than increasing domestic vaccination at preventing SARS-CoV-2 infections at home. This finding is largely driven by the effects of global travel. If a COVID-19 outbreak happens abroad, it can be introduced to, say, the United States through international travelers. However, if the U.S. population is highly vaccinated, helping other countries reach herd immunity will reduce the risk of infections coming into the country.
In an interview with Yale News, Saad Omer, director of the Yale Institute for Global Health and senior author of the study, describes the findings and what it means for countries like the United States. This interview has been condensed and edited.
In the study, you note that there has been a lot of focus on prioritizing vaccine distribution within countries, but how to allocate across countries might be a more important question. Why is that?
Saad Omer: First, it's the right thing to do to make sure everyone is vaccinated in the middle of a pandemic. But secondly, if you're trying to douse a fire, introducing new embers to it will reignite the fire again and again. Similarly, if you're trying to halt SARS-CoV-2 spread within the U.S., introducing new infections from other countries will just perpetuate the problem here. Importing infections through travel means your success at halting the spread will be under threat all the time.
What do these findings mean for countries like the United States that have not yet reached herd immunity but are experiencing slowing rates of vaccine uptake?
Omer: In these cases, it can be optimal to do both, to continue to pursue domestic vaccination and share vaccines abroad. And I think high-income countries have been a bit too slow in terms of making vaccines available to other nations and exporting vaccine production. The G7 countries—Canada, France, Germany, Italy, Japan, the United Kingdom, and the United States—announced their vaccine donations, but most are happening next year. And while the U.S. has led in vaccine donations—which have saved lives—doing a lot of good isn't always sufficient. More people have died globally from this pandemic after vaccines became available than before. High-income countries need to match the moment.
What do you hope comes from these findings?
Omer: Better policies, because as we can see from these results, sharing vaccines is rational. It is in our best interest to do it.
Does it fall to individual countries to enact these sharing policies or is there an opportunity to develop more global guidance?
Omer: We likely won't come to a global agreement anytime soon. But a reasonable approach is to strengthen COVAX, the entity established by the Coalition for Epidemic Preparedness Innovations, Gavi, and the World Health Organization. COVAX's goal is to accelerate COVID-19 vaccine development and distribution around the world. The U.S. is sending 75% of its donations to COVAX, and that's a reasonable framework for other countries to follow.
What should people take away from the findings of your study?
Omer: That vaccine equity is not a zero-sum game. You can protect the most vulnerable within your own borders while also protecting the rest of the world.
More information: Tiziano Rotesi et al, National interest may require distributing COVID-19 vaccines to other countries, Scientific Reports (2021). DOI: 10.1038/s41598-021-97544-5