Many IVF embryos not implanted due to mosaic abnormalities may be viable
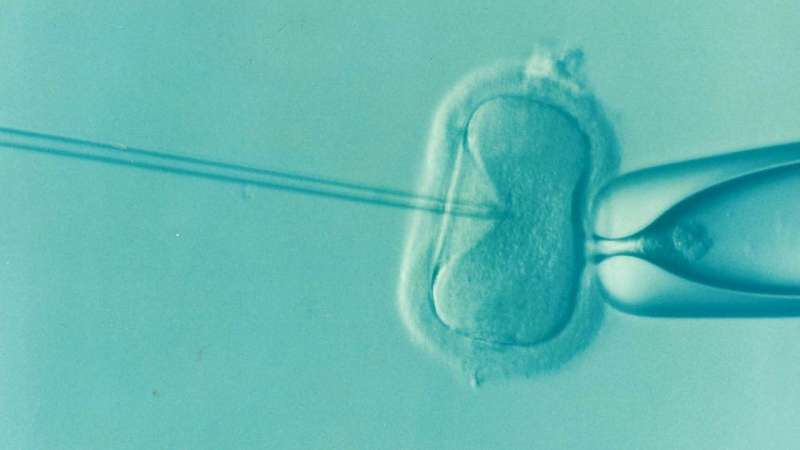
One factor that limits the success of in vitro fertilization (IVF) procedures is the number of viable embryos available for implantation in the uterus. A study published November 18 in the American Journal of Human Genetics suggests that many of the embryos that are discarded or downgraded due to chromosomal abnormalities have the potential to lead to successful pregnancies. These findings could have important implications for people undergoing IVF treatments.
"We believe the clinical data generated from this trial will resolve some of the major concerns that arise during pre-implantation genetic testing and will be of fundamental importance for helping many infertile patients make more informed reproductive decisions," says first author Antonio Capalbo, a specialist in reproductive genetics at Igenomix Italy, a company that provides genetic testing services. "This trial has the potential to drive a radical change in the clinical management of IVF and to support the development of updated guidelines and recommendation from scientific societies."
The researchers focused on the prevalence and distribution of aneuploid cells (cells with chromosome imbalances) within lab-created blastocysts, the precursor to embryos. In particular, they looked at a condition called mosaicism, in which embryos have a mix of normal and aneuploid cells. Currently, fewer than 3% of these mosaic embryos are used in IVF treatments, and several clinics in the US do not allow them to be transferred. But in many blastocysts with this type of mosaicism, the area of abnormal cells is localized to a small area that may not affect development.
In the current study, investigators conducted a double-blinded trial in which patients undergoing IVF at five hospitals in Italy had their embryos tested with pre-implantation genetic testing that looked specifically for mosaic aneuploidy. In addition to euploid embryos (those with no aneuploidy), embryos with low-grade mosaicism (20%–30% aneuploid cells) and medium-grade mosaicism (30%–50% aneuploid cells) were blindly reported as euploid and implanted. The primary outcome of the trial was defined as live birth rate, and the secondary outcome was miscarriage rate.
"It was already known that putative mosaic embryos can develop to term and make healthy babies, but many of the previous studies that looked at this issue were affected by selection bias toward a population of patients that had a poor prognosis because they had previously failed implantations with euploid embryos," he says. "Alternatively, mosaic embryos have been transferred into patients producing only aneuploid embryos, again introducing a strong selection bias toward a poor-prognosis population."
The researchers say the current study avoided that bias by being a non-selection trial, in which any embryos that fit the defined criteria were eligible for transfer. Overall, they found that across 484 euploid, 282 low-grade mosaic, and 131 medium-grade mosaic embryos, the rates of live births and miscarriages were similar. The obstetrical and neonatal outcomes were also similar.
"We did this study because we were concerned about the unmotivated dismissal of putative mosaic embryos from clinical use without robust data to support this practice," Capalbo says. "Our findings suggest that reporting mosaicism as it is currently performed doesn't provide any element of clinical utility for IVF patients. Accordingly, it seems reasonable these genetic findings not be reported after pre-implantation genetic testing, similar to what is done for variants of unknown significance in clinical genetic testing. If these findings are reported, patients should be aware that the embryos are otherwise healthy and normal."
The investigators expect that this study will immediately impact clinical practice, driving an update of guidelines and recommendations from relevant scientific societies and allowing IVF patients to improve their decision-making process when evaluating the transfer of mosaic embryos. "In the future, we encourage the preliminary use of data from non-selection trials before incorporating new pre-implantation genetic testing algorithms and aneuploidy classification criteria in routine practice," Capalbo says.
More information: Antonio Capalbo, Mosaic human preimplantation embryos and their developmental potential in a prospective,non-selection clinical trial, The American Journal of Human Genetics (2021). DOI: 10.1016/j.ajhg.2021.11.002. www.cell.com/ajhg/fulltext/S0002-9297(21)00412-2