The role of trust and knowledge in overcoming vaccination hesitancy
In examining why vaccination-hesitant people may change their minds and accept a COVID-19 vaccine, a great deal of scholarly attention and fact-checking has been devoted to what beliefs individuals hold about the coronavirus, which deceptions they've been exposed to, and how much they worry about getting sick.
But a study published online this week in the Proceedings of the National Academy of Sciences (PNAS) led by researchers from the Annenberg Public Policy Center (APPC) of the University of Pennsylvania suggests that a narrow focus on COVID-19 factors misses critical influences.
A panel study of more than 8,000 adults, surveyed over time, found that their willingness to be vaccinated against COVID-19 was anchored in background factors such as their trust of health authorities. In addition, their knowledge about vaccination in general, flu vaccination history, and patterns of media reliance "played a more prominent role" than COVID-19-specific factors such as worry about getting infected by COVID-19 in shifting them from vaccination hesitancy to acceptance.
"Trust and knowledge about vaccination are stronger predictors of vaccination than any COVID-specific factors," said lead author Kathleen Hall Jamieson, director of the Annenberg Public Policy Center. "A communication strategy focused on COVID-specific beliefs and conspiracy theories, while valuable, may be missing a piece. We need to consistently be doing everything we can to reinforce trust in health authorities, an understanding of the nature, successes, and benefits of vaccination, and habitual vaccination behavior."
Changing intentions to be vaccinated
The study found that during the early phase of the pandemic, people's intentions to get the COVID-19 vaccine steadily declined, reaching a low in September 2020 before starting to increase, up to and after the presidential election.
The study was designed to isolate factors that could account for why people who had been hesitant to be inoculated against COVID-19 became more receptive to it. To do so, researchers analyzed data from probability-based samples of U.S. adults in five states—Florida, Michigan, Ohio, Pennsylvania, and Wisconsin—gathered as part of APPC's 2020 Annenberg Institutions of Democracy Election Study. (A book about the larger data set will be published in 2022.)
The PNAS study examined data collected in eight waves of the panel survey, from July 2020 to February 2021, with a focus on attitudes shifting from September-October 2020 to January-February 2021. Within the latter four-month period, Pfizer-BioNTech and Moderna announced that their vaccines were successful, the Food and Drug Administration issued emergency use authorizations for those vaccines, and Joe Biden was elected president.
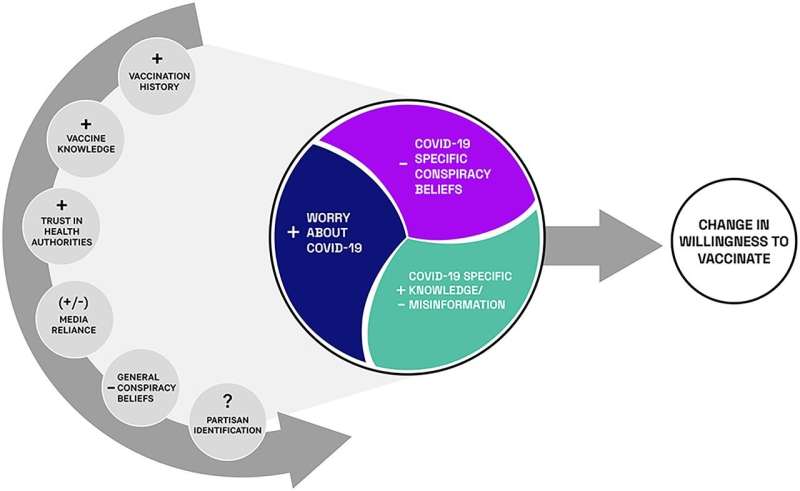
The researchers anticipated that such background factors as vaccination history, vaccine knowledge, trust in health authorities, media reliance, general conspiracy beliefs, and partisan identification would be the main determinants of a changed willingness to vaccinate and that factors specific to COVID (the influences seen in the colored circle of the model) would exert a smaller impact.
Trust and knowledge in vaccination hesitancy
The researchers found that trust in scientific institutions and health authorities was central to individuals' intentions to be vaccinated, especially in the early part of the pandemic. However, as the pandemic continued, other factors related to trust emerged.
"The more general influences on the willingness to vaccinate, as opposed to beliefs related to the pandemic itself, were really critical to understanding the change in hesitancy," said co-author Dan Romer, APPC's research director. "Background beliefs and behavior regarding vaccination in general were more than twice as predictive of the change in vaccination as beliefs about the pandemic itself, such as the threat of getting infected."
The evidence, the researchers wrote, "documents the need for the public health community to redouble its efforts to preemptively and persistently communicate not only about how vaccines in general work but also about their benefits, safety, and effectiveness." Contrary to expectations, the researchers found that general conspiracy thinking did not act as a negative predictor of people's willingness to change their thinking about getting vaccinated, though belief in specific COVID conspiracies did—suggesting the need to identify and counter health-related conspiracies as soon as they start circulating in the media.
The researchers conclude: "As the public health community asks how the disposition to accept a newly authorized vaccine can be increased before one is created in response to the next pandemic, this study suggests the importance of proactively increasing knowledge about vaccination in general while also debunking prevalent deceptions about it; deploying ongoing health interventions and messages bolstering trust in health and science authorities, especially those at the community level; counteracting misinformation in regard to conspiracy thinking/beliefs about the vaccine in question; and maximizing uptake of existing vaccines such as that for the seasonal flu."
In addition to Jamieson and Romer, the study was authored by Patrick E. Jamieson, director of the Annenberg Health and Risk Communication Institute, at the policy center; Kenneth M. Winneg, APPC's managing director of survey research; and Josh Pasek, an associate professor of communication and media at the University of Michigan and an APPC distinguished research fellow.
More information: Kathleen Hall Jamieson et al, The role of non–COVID-specific and COVID-specific factors in predicting a shift in willingness to vaccinate: A panel study, Proceedings of the National Academy of Sciences (2021). DOI: 10.1073/pnas.2112266118