Why are some viruses harmless and others deadly?

Viruses outnumber humans by about 400 trillion to one, and yet pandemics are rare. Why? Why do a few viruses inflict so much damage, when the vast majority are harmless or even helpful?
Those questions drive A.J. te Velthuis, a virologist who joined Princeton's molecular biology faculty in January 2021.
"AJ is the future of virology," said Bonnie Bassler, the Squibb Professor in Molecular Biology and chair of the department. "Our department has always been a powerhouse in virology. When it was time to bring in a new assistant professor, our senior virologists—an incredible group of scholars and intellects—helped us understand where the future of this field is going, and they pinpointed him."
"I work on RNA viruses, and I've been doing it for a very long time," te Velthuis said. "I am particularly interested in why some new viruses, when they jump over to humans, suddenly trigger severe diseases, whereas when they were in bats or in other species, they seemed almost harmless."
He studies the fundamental mechanisms for how viruses replicate and confuse our immune systems. He also works on new masks that inactivate viruses, antivirals that stop viral replication, and how variants of the same virus—such as omicron or delta—can arise and cause more harm than others. He pointed to the key role played by vaccination programs around the world.
"Unvaccinated people are acting as a reservoir from which the virus causing COVID-19 can keep jumping back into vaccinated people," te Velthuis said. "It's a perfect selection model for new variants, unfortunately."
Defanging the coronavirus
In the earliest days of the pandemic, researchers experimented on live specimens of SARS-CoV-2, the virus that causes COVID-19, at great personal risk. Te Velthuis found a way to change that—to edit the genome of the new SARS strain so that he and his colleagues around the world could study the virus without exposing themselves and their loved ones to the deadly disease.
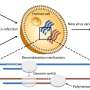
To do so, he took advantage of the fact that this is an unusually complex virus, with an elaborate blueprint coded in a long sequence of RNA (the single-stranded cousin of DNA).
The long genome can be thought of like a train, with a locomotive and a long string of cars linked together behind it. When the virus wants to give instructions to the cells it is invading, it needs to highlight the most relevant part of its genome, so it splices out that "train car" and reattaches it up front. The researchers in te Velthuis' lab used that property to isolate one locomotive and one train car, resulting in a micro-virus that cannot infect new cells but can still be useful for testing antiviral treatments and studying new mutations.
"It's not deadly anymore, because you need all the other 'train cars' to create a full, infectious virus particle," te Velhuis said. "If you just have one train car in isolation, it can't produce anything infectious, but it gives you information about how the wheels work, how strong the locomotive is."
In many ways, te Velthuis thinks like an engineer, which he says comes from a childhood filled with construction toys. "Structural biology has advanced in such a way that you can start to look at molecules almost like Legos in how they fit together and how we can build with them. It makes it a lot of fun to think about and to draw them and teach students about it. It's so visual, and so, so beautiful."
That love of looking at these tiny structures was part of what drew him to Princeton, with its extraordinary community of microscopy researchers. "An image tells so much more than some of the biochemical work that we do—both to scientists and when communicating with students and the wider community," te Velthuis said. "So getting to work with them and finding new ways to look at viruses is really inspiring."
He arrived at Princeton in January 2021 to find a mountain of boxed equipment and a construction zone where his lab should be. He already had one graduate student, Kimberly Sabsay, who he co-advises with Ned Wingreen, Princeton's Howard A. Prior Professor in the Life Sciences, who is also a professor of molecular biology and the Lewis-Sigler Institute for Integrative Genomics.
Sabsay and te Velthuis had the struggle—and joy—of building the lab from scratch, despite COVID-related construction delays and supply challenges.
"Unpacking the boxes of new equipment felt like Christmas, and that kept us sane as delay after delay prolonged construction," Sabsay said. "The experience I got, working one-on-one with A.J. to design and put together his dream lab, was invaluable. The process was painfully slow, riddled with frustration and failure, but it ultimately proved to be more rewarding than I could have ever imagined—much like science itself."
A swab to predict pneumonia?
Long before the current pandemic, te Velthuis studied coronaviruses as well as various strains of influenza, comparing a seasonal flu (H1N1) with two pandemics: the 1918 flu and the avian flu (H5N1). While the seasonal flu usually causes mild symptoms, the other two flus can trigger an overreaction from the immune system that fills the lungs with fluid (pneumonia). As the world learned in early 2020, the coronavirus family of viruses has a similar pattern: While most coronaviruses only cause mild cold symptoms, some can cause pneumonia, including SARS-CoV-2.
Te Velthuis and his team found that the molecular trigger that turns the flu into pneumonia is a tiny viral RNA molecule. They can detect it in vitro, in ferrets infected with the 1918 flu, and in saliva swabs from hospital patients; continued research, te Velthuis hopes, could lead to a rapid test to predict severe influenza, ultimately resulting in faster and better treatment.
He wants to take it a step further, as well. His team is now working to discover the mechanism behind this trigger, with a goal of finding medicines that inactivate this process, transforming a severe health threat into a minor inconvenience.
"If we can have a tool, a drug for instance, that we can use when a pathogenic virus comes around, we can immediately turn it into a more manageable seasonal virus, and we wouldn't see as much pressure on hospitals and other healthcare institutes," said te Velthuis, whose work is partially funded by the National Institutes of Health. "That's the bigger dream, the bigger goal."
Teacher and researcher
This spring, te Velthuis will teach "Pathogens, Pandemics and Technologies" with Cameron Myhrvold, also an assistant professor of molecular biology.
The course will examine pandemics from multiple angles, te Velthuis said. "How do you study a virus? How do you develop ways to protect yourself against it? What does a virus need to get into a cell? What makes them cause disease? What causes a pandemic?"
Viruses are very different from each other, but they all have to solve the same problems, te Velthuis explained—getting into cells, interacting with proteins, evading immune defenses—which means viruses often use similar mechanisms. That's part of why he's so excited to join Princeton's research community. "The virus is trying to solve engineering problems as it jumps between environments, so it's really helpful to hear how physicists and engineers think about these things," he said.
It's no coincidence that Princeton's two newest coronavirus researchers are teaching a course on pandemics, of course.
"In the Department of Molecular Biology, we put a premium on being excellent teachers, in every manifestation of that role—in the classroom, in the lab, with thesis students," said Bassler, the department chair. "In our department, many students become co-authors on published papers, because they make central discoveries in their senior thesis work. Student research in the Princeton molecular biology department is the real deal. We have total immersion in research and in the thrill of discovery—we don't kid around about that here."
"A.J. gives us the freedom to cook up our wildest experimental dreams," said Sabsay, who has continued in his lab. "And when our delirious plans lead us to failure, he is right there with us to help resuscitate them and keep our fantasy alive for as long as possible."
"A.J. never says no to anything I want to try," agreed Elizaveta Elshina, who was his first graduate student and came with te Velthuis from Cambridge University.
"Science is all about trying different things," said Karishma Bisht, a postdoctoral researcher who joined his lab in fall 2021. "Not everything is going to work, but you wouldn't know it unless and until you try it—and AJ is willing to take the risk with you to explore these scientific questions by sharing his knowledge, expertise and resources."
Bassler said that te Velthuis has already made himself a valuable addition to his many communities of researchers—within his lab, within their department, and across the University. "Because of our commitment to teaching, Princeton self-selects for people who believe that part of the social contract of the scientist is to teach the next generation of scientists to be scientists," she said. "And A.J. is already contributing to our department's collaborative, nurturing spirit of "All for one and one for all." That happened fast, especially given the COVID restrictions. It's hard to immerse yourself into a department on Zoom, but he did it."