New study reveals why HIV remains in human tissue even after antiretroviral therapy
Thanks to antiretroviral therapy, HIV infection is no longer the life sentence it once was. But despite the effectiveness of drugs to manage and treat the virus, it can never be fully eliminated from the human body, lingering in some cells deep in different human tissues where it goes unnoticed by the immune system.
Now, new research by University of Alberta immunologist Shokrollah Elahi reveals a possible answer to the mystery of why infected people can't get rid of HIV altogether.
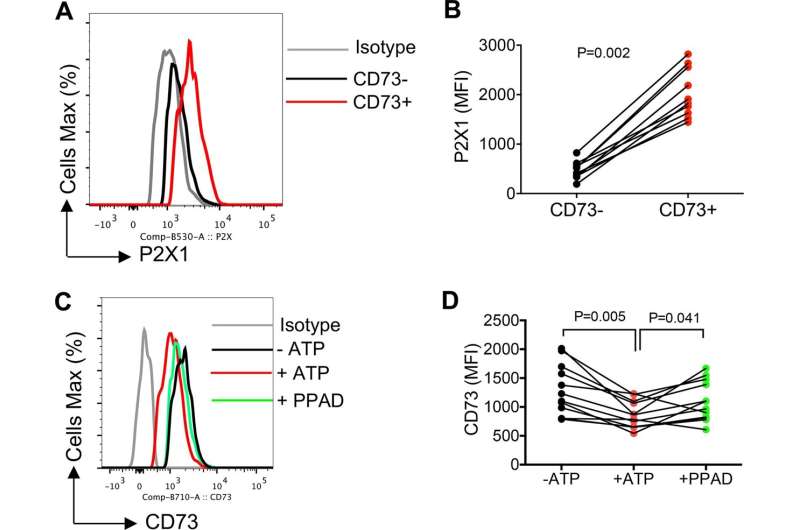
Elahi and his team found that in HIV patients, killer T cells—a type of white blood cells responsible for identifying and destroying cells infected with viruses—have very little to none of a protein called CD73.
Because CD73 is responsible for migration and cell movement into the tissue, the lack of the protein compromises the ability of killer T cells to find and eliminate HIV-infected cells, explained Elahi.
"This mechanism explains one potential reason for why HIV stays in human tissues forever," he said, adding that the research also shows the complexity of HIV infection.
"This provides us the opportunity to come up with potential new treatments that would help killer T cells migrate better to gain access to the infected cells in different tissues."
After identifying the role of CD73—a three-year project—Elahi turned his focus to understanding potential causes for the drastic reduction. He found it is partly due to the chronic inflammation that is common among people living with HIV.
"Following extensive studies, we discovered that chronic inflammation results in increased levels of a type of RNA found in cells and in blood, called microRNAs," he explained. "These are very small types of RNA that can bind to messenger RNAs to block them from making CD73 protein. We found this was causing the CD73 gene to be suppressed."
The team's discovery also helps explain why people with HIV have a lower risk of developing multiple sclerosis, Elahi noted.
"Our findings suggest that reduced or eliminated CD73 can be beneficial in HIV-infected individuals to protect them against MS. Therefore, targeting CD73 could be a novel potential therapeutic marker for MS patients."
Elahi said the next steps in his research include identifying ways the CD73 gene can be manipulated to turn on in patients living with HIV and off in those with MS.
The study is published in PLOS Pathogens.
More information: Shima Shahbaz et al, Elevated ATP via enhanced miRNA-30b, 30c, and 30e downregulates the expression of CD73 in CD8+ T cells of HIV-infected individuals, PLOS Pathogens (2022). DOI: 10.1371/journal.ppat.1010378