Discovery of gene defect for allergy and autoimmune diseases

An international team led by a physician from the Karl Landsteiner University for Health Sciences, Krems, describes for the first time a mutation of the IL-33 gene in the human genome that results in multiple allergic disease manifestations, and autoimmune disease.
Inflammation of the skin and the esophagus, food allergy and asthma are just some of the symptoms of a now 12-year-old boy who was the first identified to have a mutation on the IL-33 gene. An international team led by a physician from the Karl Landsteiner University for Health Sciences, Krems, discovered this new disease entity. Their description of a single case provides completely new insights into the in vivo functions of IL-33, which is considered a central upstream regulator of human immune responses. So far, studies on its function were limited to human derived in vitro cellular or animal models. This discovery of an overexpression of IL-33 in humans helps to gain new insights in the consequences of its dysregulation in humans. Concomitantly, it also opens up potential therapeutic options for affected patients.
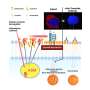
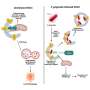
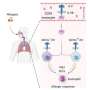
The human body's type-2 immune response serves to defend against larger pathogens, but also represents the hallmark of allergic inflammation. Interleukin 33 (IL-33), a so-called "alarmin" due to its release upon cellular damage, plays a central role in the initiation and regulation of allergic inflammation. Animal models in which its production is genetically up- or down-regulated have contributed to the understanding and suggested functions beyond allergic inflammation—but they allow only limited insight into the conditions in humans. Disease symptoms of a patient with a duplicated IL-33 gene now provide such insight for the first time.
An international team at The Hospital for Sick Children led by Prof. Thomas Eiwegger of the Karl Landsteiner Private University for Health Sciences Krems (KL Krems) succeeded in stating the diagnosis and providing the first description. "One of the most striking symptoms of the patient is chronic inflammation of the esophagus, an eosinophilic esophagitis, as well as chronic inflammatory changes of the skin," explains Prof. Thomas Eiwegger, who recently became head of the Department of Pediatrics and Adolescent Medicine at St. Pölten University Hospital, which is part of KL Krems.
Thus, a high number of eosinophilic granulocytes (hypereosinophilia), elevated levels of IgE antibodies and recurrent eosinophil-dominated inflammation of the skin occurred. According to Prof. Eiwegger: "Especially the skin reactions and the inflammation of the esophagus confirm the central role of IL-33 in type-2 immune reactions in tissues exposed to the external environment." Additionally, food allergies and asthma, as well as inflammatory complications of the broader gastrointestinal tract, also show up in terms of an autoimmune response.
Numerous investigations in the study, now published in Gastroenterology, were conducted at The Hospital for Sick Children in Toronto, Canada, in conjunction with the university there. In addition to the inflammatory symptoms, physical abnormalities of the patient were also recorded. These include changes in the cranial bones, the jaw and the face, as well as delayed weight gain and growth in length with hypermobility of the joints, short-sightedness and a moderate developmental delay. For Prof. Eiwegger, these are indications of the pleiotropic role of IL-33 beyond classical type-2 inflammation.
More gene, more cytokine
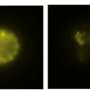
The extent to which this gene duplication affected the actual concentration of the cytokine IL-33 in the blood and various tissues was very interesting. Although there was no increase in IL-33 in the blood, there were significant increases in the tissues of the gastrointestinal tract as well as the skin. "The different subcellular localizations of IL-33 in different tissues were also striking," notes Prof. Eiwegger. "For example, it showed up in the nucleus in inflamed skin tissue, but in the cytoplasm in inflammation-free intestinal tissue." The team suggests that these results show how tightly IL-33 is regulated locally and points to new explanations for the patient's tissue-specific disease patterns that could be critical for targeted therapies for diseases in which IL-33 plays a role.
Monoclonal antibodies that bind and remove IL-33 are being investigated as therapeutic options in phase 2 studies for the treatment of asthma, atopic dermatitis and food allergies—an option that the team also considers worth evaluating here. Thus, this research exemplifies modern precision medicine in which basic science directly impacts clinical decision making.
More information: Ashish K. Marwaha et al, A Chromosomal Duplication Encompassing Interleukin-33 Causes a Novel Hyper IgE Phenotype Characterized by Eosinophilic Esophagitis and Generalized Autoimmunity, Gastroenterology (2022). DOI: 10.1053/j.gastro.2022.04.026