The pandemic accelerated decades of research, leading to inhaled vaccine candidate for COVID-19

No one wanted COVID-19. The pandemic has created misery, death and hardship, and it isn't finished yet.
Still, the lingering crisis has generated opportunities, by expediting research that may benefit humanity far beyond the pandemic. Inhaled vaccines are one example. I am part of a multidisciplinary team working to make these a practical reality, much sooner than would have been the case without the pandemic.
We are now in the early stages of testing a next-generation COVID-19 vaccine that our earlier research in animals suggests will last longer, be more effective and stand up well to future variants of the COVID-19 virus.
Before COVID-19 emerged, my colleagues and I at McMaster University were working to develop a new inhaled form of vaccine delivery that could finally take on one of the most challenging respiratory infections: tuberculosis, still a scourge in low- and middle-income countries and in remote areas. In Canada it disproportionately affects people living in Inuit Nunangat and First Nations living on reserve.
After decades of work, progress was steady, but slow. The lack of urgency to solve a problem that mainly affects people living in poor conditions had made it difficult to generate the resources and momentum needed to complete our research.
The urgency of COVID-19
The COVID-19 pandemic, being truly global, created the demand for vaccines, such as the now-familiar ones from Pfizer, Moderna and AstraZeneca. These vaccines have got us through the immediate crisis, as the virus was spreading rapidly, and have served us well, preventing serious illness and death in countries where vaccines were available.
These vaccines represent great strides, but they are not as effective in all populations, nor are they as robust against new variants as they are against the original strain of SARS-CoV-2, the virus that causes COVID-19.
Our research suggests that the next-generation COVID-19 vaccine we are currently testing will be more effective for longer, and will protect against new variants.
Our team, which includes experts in pathology and molecular medicine, infectious diseases, immunity and aerosol particles, has taken the progress we'd made toward a tuberculosis vaccine and quickly adapted the same approach to COVID-19. This delivery system can be transformative.
This promising science presents an opportunity to make a lasting and wider impact beyond COVID-19. While we still need to understand more fully how these vaccines work, my colleagues and I are optimistic this will finally give us a step up in controlling tuberculosis and other lung infections.
An inhaled COVID-19 vaccine
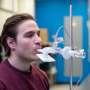
We are conducting human trials of our new COVID-19 vaccine. The Phase 1 clinical study is evaluating safety, as well as testing for evidence of immune responses in the blood and lung. Our new multivalent vaccine, manufactured for our clinical trial in the Robert E. Fitzhenry Vector Laboratory, targets multiple viral proteins, both the spike protein on the surface and proteins inside the virus.
With new variants, mutations occur in the spike protein on the outside of the virus. This makes the current vaccines less effective because they target only the spike protein. However, other proteins inside the virus stay the same. Targeting multiple proteins means that if clinical trials show that our multivalent COVID vaccine is effective, it will still protect against infection with new variants as they come along.
In addition to being a friendlier way to take a vaccine, the inhaled form requires much less vaccine—as little as one percent of what is currently being used in the present vaccines.
The new process delivers the vaccine directly to where the body will use it: the mucosal surface of the airways. This means less waste and more benefit, lower costs and reduced side-effects.
The vaccine triggers an immune response in the cells lining the lungs to directly protect against COVID-19. This mucosal vaccination could also protect against other respiratory infections, from the common cold to influenza and bacterial pneumonia by rapidly calling on a range of immune cells that are at the ready as the first line of defence against infection. This lasting and broad form of general protection against infection is called innate immunity.
When the virus particles in the vaccine are taken up by immune cells in the lung, they recruit more cells from elsewhere in the body and together they generate a strong immune response. The process involves a very beneficial type of cell called memory T cells, which, once recruited and activated, stay in the lung, and remain ready to face the infection.
Decades of research
Our multidisciplinary team has arrived at the threshold of introducing this potentially transformative vaccine by pivoting decades of research. The antecedent of this work, the development of the viral vector, dates back more than 50 years to the work of molecular biologist Frank Graham, who created a microscopic Trojan horse by using a human adenovirus to carry critical viral genes safely into the body.
If we are able to show the new inhaled vaccine is safe and effective, as we anticipate, the payoffs can be huge in terms of human health, medical costs and better quality of life overall, especially for vulnerable populations. We are hopeful that greatly reduced costs for production, storage and shipping of the new vaccine product will allow greater access in developing and remote areas.
No one wanted this pandemic, but when at last it's over, a new generation of vaccines targeting lung infections means we may all be able to breathe again, in all senses of the expression.
This article is republished from The Conversation under a Creative Commons license. Read the original article.![]()