Robotic bronchoscopy shows promise to improve lung biopsies, new analysis shows
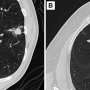
Lung nodule biopsies performed with new robotic bronchoscopy technology may be safer and more effective than those done by traditional methods, a study by researchers at University of Texas (UT) Southwestern suggests.
UT Southwestern was the first medical center in Dallas-Fort Worth—and among the first in the country—to use robotic-assisted bronchoscopy (RAB) to biopsy pulmonary lesions. Paired with advanced imaging that provides real-time 3D visuals, the technology enables UTSW's Interventional Pulmonology team to navigate an ultra-thin, ultra-flexible tube with light and camera capabilities into a patient's lungs to pinpoint and test suspicious abnormalities.
The increased dexterity of the steerable tube makes it possible to safely reach areas in the lungs that couldn't be accessed through traditional bronchoscopy and other sampling tools.
A retrospective analysis of 200 of those procedures—the largest cohort studied to date—found that shape-sensing, robotic-assisted bronchoscopy (ssRAB), when combined with technologies such as intra-procedure cone beam CT imaging (CBCT) and radial endobronchial ultrasound, offers high diagnostic accuracy, sensitivity, and specificity with an excellent safety profile. The findings were published in Lung.
"The goal of advanced bronchoscopy is to diagnose lung nodules and perform mediastinal staging in a single procedure, while achieving a comparable diagnostic yield to percutaneous biopsy and at the same time, minimizing complications," said Kim Styrvoky, M.D., Assistant Professor of Internal Medicine in the Division of Pulmonary and Critical Care Medicine at UT Southwestern, and Muhanned Abu-Hijleh, M.D., Professor of Internal Medicine in the Division of Pulmonary and Critical Care Medicine. Drs. Styrvoky and Abu-Hijleh are members of the Interventional Pulmonary section at UTSW and the Harold C. Simmons Comprehensive Cancer Center.
"The diagnostic yield of current bronchoscopic techniques is limited, and there is about a 1 in 4 chance of pneumothorax, or collapsed lung, with percutaneous biopsy," Dr. Styrvoky said. "Our study showed that this new technology provided accuracy of 91.4%, on par with traditional biopsy methods, while reducing the risk of pneumothorax complication to 1%."
Lung cancer remains the leading cause of cancer-related deaths for both men and women in the U.S. Each year, between 1.5 million and 2 million pulmonary nodules—spots or related abnormalities—are identified through diagnostic imaging. UT Southwestern is using robotic bronchoscopy in cases where traditional biopsies present a higher risk of complications, including patients with lesions deep in the lung, near major blood vessels, or adjacent to a portion of diseased lung.
This was UTSW's first reported study detailing the usage of ssRAB-CBCT, but other trials focusing on various aspects of robotic bronchoscopy are underway.
If further studies confirm the findings, ssRAB-CBCT has the potential to become the standard of care for targeted lung sampling, Drs. Styrvoky and Abu-Hijleh said.
Other UTSW researchers who contributed to this study include Audra Schwalk, David Pham, Hsienchang T. Chiu, Kristine Madsen, Stephen Carrio, Elizabeth M. Kurian, and Luis De Las Casas.
More information: Kim Styrvoky et al, Shape-Sensing Robotic-Assisted Bronchoscopy with Concurrent use of Radial Endobronchial Ultrasound and Cone Beam Computed Tomography in the Evaluation of Pulmonary Lesions, Lung (2022). DOI: 10.1007/s00408-022-00590-7