This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
trusted source
proofread
Q&A: New guidance states breast cancer screenings should now begin at age 40
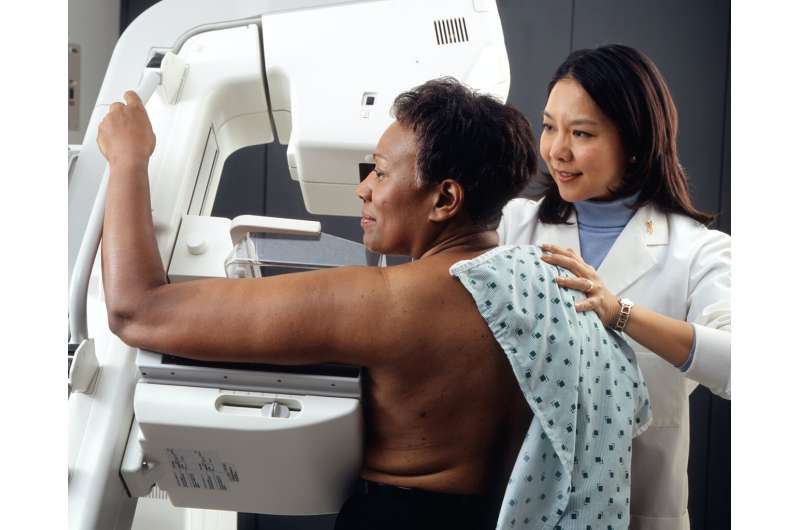
If you're a person who gets breast exams, listen up. According to new guidance from medical experts, routine mammograms should now begin at 40 years old—10 years earlier than previously recommended.
The proposal comes from the U.S. Preventive Services Task Force, which released the new screening guidelines based on consistently high rates of breast cancer among women under 50 years old. Black women in particular are more likely to have breast cancer at earlier ages and with a worse prognosis than white women.
For decades, researchers have been trying to figure out why. Among them is Boston University cancer epidemiologist Julie Palmer. She studies aggressive types of breast cancer that disproportionately impact young Black women and supports the recommendation for starting mammograms at a younger age.
"It's better to err on the side of starting mammographic screening early in order to detect cancer in young women," says Palmer, the BU Chobanian & Avedisian School of Medicine Karin Grunebaum Cancer Research Professor. "Those cancers are more likely to be aggressive."
She helped start BU's Black Women's Health Study (BWHS) in 1995. The biggest and longest-running epidemiologic study of Black women ever conducted, it has helped arm health care professionals and researchers with knowledge specifically related to a community that's historically overlooked in research and medical studies. In a 2021 paper, the team found that out of 50,543 women from 1997 to 2017, 2,311 of them experienced breast cancer. Based on other findings from BWHS, Palmer and a team of researchers developed a risk prediction model for clinicians to identify women at higher than average risk of breast cancer. This can inform recommendations made by primary care providers to refer patients for genetic testing, or to start regular mammograms early or more frequently.

In light of the new breast cancer screening recommendations, The Brink spoke with Palmer about the increasing risk of breast cancer in young women, the significance of the change in clinical guidelines, and why regular screenings are an important part of routine health care.
The Brink: As a researcher in this field, what was your reaction to the new recommendations?
Palmer: I was pleased to hear about it. There have been different guidelines at different times, and the task force previously recommended starting at age 50 and older. Changing it to having mammograms every other year starting at age 40, I think is correct.
Is starting regular mammograms 10 years early a significant change?
I like the recommendation because then women will not only get their first mammogram earlier, but as part of having a mammogram, they will be asked a series of questions about family history and other factors. That will help to define whether the person is in a high-risk category and should be screened more often.
Why are regular mammograms an important aspect of primary health care?
Mammograms are the cheapest, least invasive way to detect tiny tumors that can't be felt. They're good, but not perfect. For some women, depending on the breast density, it may be harder to visualize those tiny tumors with a mammogram. Those women might be referred for a breast MRI, which is a different modality, typically only recommended for high-risk women or for special reasons. But a mammogram is the number one way to go for the average woman.
Why are rates of breast cancer increasing among younger women?
Rates aren't increasing very much, but they're certainly not going down as some other cancers are. This means that it likely has to do with modifiable factors among the U.S. population. For postmenopausal women, being very overweight slightly increases their risk, and we know that has been an increasing problem. Another factor could be alcohol intake—it's unclear how much alcohol patterns have changed among women over time, but alcohol is one of the modifiable risk factors for breast cancer. Another possible reason for rates going up a little bit in the U.S. is lack of physical activity. We know that's been a problem in this country for several decades. Women who had more vigorous exercise—it's not clear if it's in early life or throughout the lifespan—seem to have a somewhat reduced risk of breast cancer.
What have we learned over the years about risk factors related to breast cancer? What puts some people at higher risk?
In general, the risk increases with age up to the early 70s. There are two main molecular subtypes of breast cancer. The cancers that are hormone responsive, which are the majority of cancers in any population group, are called estrogen receptor–positive. It's also the most treatable type, and it tends to be a little bit less aggressive. We also know more about the factors that increase risk, because it is hormone related. Some risk factors—like higher body mass index, taking hormones, and alcohol use—are more associated with hormone receptor–positive breast cancer. The other main subtype, hormone receptor–negative, which is less common, tends to be more aggressive, occurs at younger ages, and more often in Black women relative to all other population groups in the U.S.—and we don't know why that is.
Do we have any idea why Black women are more likely to get breast cancer at a younger age?
It hasn't been so easy to figure out what factors influence the risk—all factors for breast cancer have a small association with risk, compared to smoking and lung cancer when, if you smoke, you have seven times the risk. One factor that doesn't get talked about much but has been shown in a number of studies, including our own, is dietary intake. Studies indicated that women who ate a diet higher in fruits and vegetables have a reduced risk of this aggressive type of breast cancer. It's also possible that women who have type 2 diabetes, which causes increased inflammation, may have a higher risk of that type of cancer.
We've also learned that breastfeeding slightly protects the mother against later breast cancer. Studies, including our own, have found that women who have had more than one baby and didn't breastfeed, are at a higher risk of estrogen receptor–negative breast cancer relative to women who didn't have any babies. And that's the opposite of what we know for the more common type of breast cancer—women who have had babies have a lower risk of breast cancer compared to women who've never had a baby. It's tricky because breastfeeding isn't always a choice. There are lots of reasons to breastfeed, but it can be exceedingly difficult for some women, because of their biology and their economic situation, their job situation.
What influenced you starting the BWHS?
It came from realizing that there was very little health research being done in the Black population, among Black women. My previous research had all been on women's health and I had the model for the study from the Nurses' Health Study, but that was almost entirely white women. We really needed a similar study of Black women so that we could study not just cancer, but also all of the other health conditions that are more common in Black women.