This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
trusted source
proofread
Analysis of the 2022 mpox virus using human keratinocytes and human iPS cell-derived colon organoids
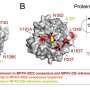
![Characterization of the MPXV-infected keratinocytes. Human keratinocytes were infected with MPXV (0.05 PFU/cell) and subjected to RNA-seq analysis. (A) Phase images of uninfected and MPXV-infected keratinocytes. (B) Immunofluorescence analysis of MPXV protein (green) and KRT10 (red) in uninfected and MPXV-infected keratinocytes. Nuclei were counterstained with DAPI (blue). (C) A volcano plot of differentially expressed genes in uninfected and infected keratinocytes (log2 fold-change >2.5, adjusted p-value [padj] Analysis of the 2022 mpox virus using human keratinocytes and human iPS cell-derived colon organoids](https://scx1.b-cdn.net/csz/news/800a/2023/analysis-of-the-2022-m.jpg)
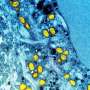
A research team led by Junior Associate Professor Kazuo Takayama (CiRA, Kyoto University) and Professor Kei Sato (Institute of Medical Science, The University of Tokyo) experimentally infected human keratinocytes and human iPS cell-derived colon organoids with mpox virus (MPXV) and characterized the virology of the conventional MPXV strain and the 2022 outbreak strain (2022 MPXV). The results were published in the Journal of Medical Virology on June 6, 2023.
Since the first identified case of mpox in the Democratic Republic of Congo in 1970, cases of mpox have been observed repeatedly in the Middle East and Africa. In 2022, however, a new strain of MPXV (2022 MPXV) emerged and has now spread beyond the typical affected areas and to different parts of the world. MPXV is classified into three strains, clade I, IIa, and IIb. Notably, 2022 MPXV belongs to clade IIb and is known to be less lethal than clade I.
While the clinical manifestations of mpox include rash, fever, headache, and lymphadenopathy, infection with 2022 MPXV is known to cause a rash, particularly in the rectal and genital areas. However, there has yet to be an in-depth comparative analysis of virological characteristics among the MPXV strains. Furthermore, considering that clinical presentations of 2022 MPXV differ substantially from the other strains, a detailed analysis of 2022 MPXV is necessary.
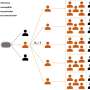
In this study, the group infected human keratinocytes and human iPS cell-derived colon organoids with the three known strains of MPXV, Clade I, Clade IIa, and Clade IIb, and evaluated their infectivity and host responses. All three viral strains were found to infect keratinocytes and colon organoids. In particular, keratinocytes showed approximately 7–42 times higher infection efficiency when compared to colon organoids.
The researchers also observed MPXV infection to cause keratinocyte dysfunction and mitochondrial damage. Furthermore, while keratinocytes infected with 2022 MPXV showed increased expression of genes associated with hypoxia, human iPS cell-derived colon organoids infected with a clade I strain primarily showed intestinal dysfunction.
Although several therapeutic agents targeting MPXV viral proteins have already been developed, there are still ongoing efforts to examine their antiviral effects in human cells. As such, in addition to antiviral drugs, this infection model may be used to evaluate potential therapeutic agents that act directly to prevent damage to the skin and colon.
Furthermore, as with severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), MPXV has the potential to acquire new mutations, thereby requiring further development of preventative drugs or antivirals in the future. The research team hopes these findings will lead to a better understanding of MPXV and facilitate the development of MPXV therapeutics.
More information: Yukio Watanabe et al, Virological characterization of the 2022 outbreak‐causing monkeypox virus using human keratinocytes and colon organoids, Journal of Medical Virology (2023). DOI: 10.1002/jmv.28827