This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
reputable news agency
proofread
A Philadelphia surgeon is a leader in robotic heart surgery. Why aren't more following?

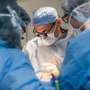
Cardiothoracic surgeon Francis Sutter sits in a corner of a darkened operating room at Lankenau Medical Center, his head buried in what looks like a large virtual-reality headset.
His hands are nowhere near the chest of the patient that he is operating on. Instead, he uses joysticks to control a robot making precise cuts near the beating heart.
The setup resembles a video game, but no game has stakes this high. "One false move with the robot arm, and you put a hole in the heart," he said.
The procedure to replace a clogged artery with a new one, known as coronary artery bypass graft, or CABG, is the most commonly performed heart surgery in the U.S. But the method that Sutter is using is uncommon. Only 1% of CABG surgeries nationwide in the past five years were performed using a robot, according to data from the Society of Thoracic Surgeons. More than 200 of the roughly 1,800 robotic CABGs in the U.S. in 2021 were performed in Lankenau, where Sutter serves as chief of cardiac surgery.
Although robots are becoming more familiar in some cardiac procedures, many surgeons question whether the robot-assisted method is an improvement when it comes to the CABG procedure.
Sutter says that for patients who qualify, this type of surgery spares them from an open procedure that involves breaking the chest bone and usually stopping the heart, and leaves a 6-to-8-inch scar. Instead, he said, his patients go home with three small incision scars, the largest less than two inches long.
Critics of the robotic approach, including some other top Philadelphia surgeons, say that many CABG patients needs multiple bypasses, and that's often not possible with Sutter's technique. Scary as it sounds to stop a heart, it's not risky in the hands of skilled practitioners. And the robot may add more cost, they say.
Sutter has heard the criticism. He still hopes his research will encourage more surgeons to embrace the robotic procedure that he has been doing for nearly two decades.
A steep learning curve
In 1986, Sutter began performing coronary bypass surgeries using the standard approach, though it struck him as violent and risky.
"Do you think you would like to have that?" he asked.
So Sutter was immediately interested when he heard that some surgeons around the world—mostly outside the U.S. at first—started to use a robot for the procedure in the late 1990s.
He saw a tool that allowed surgeons to operate on a beating heart, avoiding that fraught moment of praying the organ would restart. He thought robotic surgery could reduce recovery time and enable him to operate on frail patients unable to withstand the traditional surgery.
To learn how to use the da Vinci Surgical System, Sutter visited the few surgeons across the U.S. then performing the technique. He trained on pigs, dogs, and human cadavers. On living human patients, he gradually started using the robot.
"I didn't feel the least bit confident until I had at least 300 cases," Sutter said.
He started performing the procedure 18 years ago, and still marvels at how quickly his patients are sitting up in bed, just hours after the operation and not the day after.
A specialized procedure
Sutter uses the robot to address blockages in the largest artery that feeds blood to the heart muscle, in a two-part surgery that takes about four hours.
First, Sutter uses the robot to "harvest" the left internal mammary artery, the standard choice to replace this damaged artery in many CABG procedures.
Then he scrubs in, donning a sterile gown, and by hand stitches the "spare" artery to the heart, allowing blood flow to bypass the clog. This step requires the largest of the incisions he will make, a roughly 2-inch cut.
In the past, Sutter was able to do the entire surgery robotically. But the company that manufactures the robot stopped making a critical instrument for the procedure due to lack of demand.
Sutter surgically fixes only one artery in about 80% of his patients, he said. Because people often have more blocked vessels, many of Sutter's patients also receive stents—a device resembling a spring that is inserted through a catheter—in other vessels. He prefers this practice to opening the chest and performing multiple bypasses when possible. He makes the decision with a cardiologist.
The 1% vs. the 99%
Hospitals often chase cutting-edge treatments, even when the research doesn't entirely support the price tag. But heart surgeons in the Philadelphia area aren't following Sutter's robotic method.
"There's a lot of talented heart surgeons," said Rohinton Morris, chief of cardiac surgery at Thomas Jefferson University Hospital, in an interview. "There's a reason they don't do this."
Morris said the concern over the use of a heart-lung machine is outdated. About 90% of the CABG surgeries at Jefferson are on a stopped heart, and none use the robot. Randomized control trials demonstrated that performing CABG "off-pump" doesn't lead to better outcomes.
"Every heart starts back up," he said.
Temple University Hospital doesn't perform robotic-assisted CABG either, according to Yoshiya Toyoda, chair of cardiovascular surgery. His biggest concern with the robotic technique is that it limits the number of arteries that the surgeon can fix, or revascularize, in favor of propping arteries open with stents. Toyoda usually fixes four arteries in one operation, and sometimes as many as eight.
"Better skin incision vs. complete revascularization—which is better?" he asked. "I think the patient will benefit with complete revascularization."
There are also other minimally invasive techniques that allow for smaller incisions that don't involve the robot, Toyoda said.
The Hospital of the University of Pennsylvania and Penn Presbyterian Medical Center use the robot for about 10% of the approximately 550 CABG procedures the hospitals combined perform annually, a Penn Medicine spokesperson said.
Surgeons also raised concerns about costs—the robot alone is about $2 million—and the ability to train surgeons to Sutter's level of expertise. Even some experienced robotic heart surgeons don't feel comfortable using it for CABG.
T. Sloane Guy chaired the robotic surgery task force of the Society of Thoracic Surgeons for years. His specialty is mitral valve repair and 98% of the time he does them robotically. But when he performs a CABG, he does it the old fashioned way.
The procedure Sutter uses "is for the sort of super elite who dedicate themselves to it," said Guy, the director of minimally invasive & robotic cardiac surgery at the Georgia Heart Institute.
But Guy, who trained and worked in Philadelphia, is bullish about the future of robotic heart surgery. As technology improves, he believes it will become the norm because of demand from patients.
"Speedy recovery and minimally invasive is something that is important to patients," he said.
Promising data
Sutter recognizes the steep learning curve is a drawback to robotic bypass surgery.
But he believes the surgery should be an option for patients who can benefit, and that research involving his patients will show why. One of his students, surgeon Aleksander Dokollari, presented preliminary analysis of nearly 2,400 robotic CABGs performed at Lankenau in the recent Society of Thoracic Surgeons conference. They view the results, which have yet to be peer-reviewed and published, as promising.
Studies by researchers from outside of Lankenau have also demonstrated safety, and suggested positive outcomes.
But so far none used a randomized controlled trial—the gold standard of medical research—to evaluate the robotic technique against the traditional surgery.
Meanwhile, Sutter is convinced he is where he should be, inside his operating room, looking into a screen that shows the heart in 3D and magnified 10 times, while robotic arms operate a few feet away.
2023 The Philadelphia Inquirer.
Distributed by Tribune Content Agency, LLC.