This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
trusted source
proofread
Anesthesiologists should play bigger role in perioperative care of people with substance use disorders, say researchers
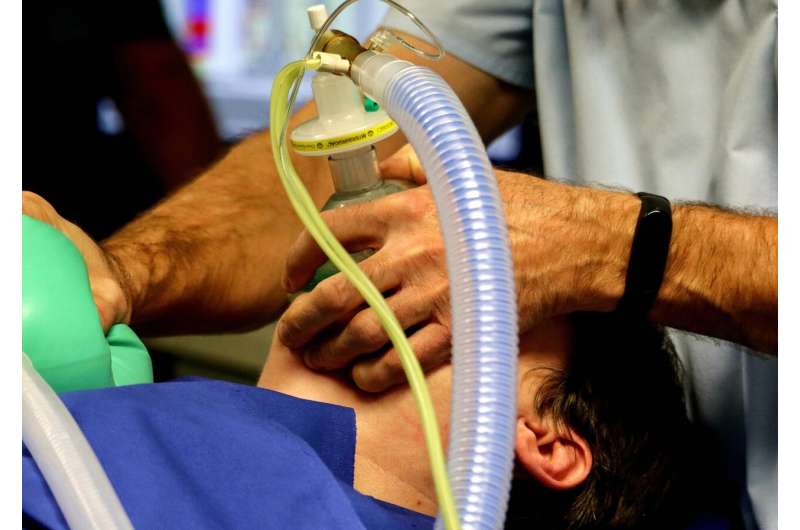
As use and misuse of alcohol, opioids, and psychostimulants continues to increase, anesthesiologists can become a more integral part of the care team managing patients with a substance use disorder (SUD), according to a series of three articles published in the September issue of Anesthesia & Analgesia.
The articles provide an overview of SUDs specific to the anesthesiologist and offer insights into pain management for opioid use disorder and exposure to psychostimulants.
"The series is timely because the fundamental philosophies that guide management of patients with SUDs have evolved rapidly over the past decade. How can anesthesiologists begin to more adequately address the unmet needs of patients with SUDs in the perioperative period?" asks Akash Goel, MD, MPH, Department of Anesthesiology and Pain Medicine, University of Toronto, and Wiplove Lamba, MD, Department of Psychiatry University of Toronto, in an editorial overview of the series.
Recommendations for expanded involvement in managing patients with SUDs
As management of SUDs has evolved, anesthesiologists have become increasingly recognized as necessary to that management. The series ask readers to look at SUDs and SUDs treatment through the lens of a wide range of biopsychosocial factors and encourages a broader approach to effective disease management. For example, one article points out how discontinuing buprenorphine, a commonly used analgesic for reducing cravings, may actually increase opioid use during the perioperative period.
Goel and Lamba offer recommendations for how anesthesiologists can contribute meaningfully to improving outcomes for patients with a SUD. Trauma-informed patient care is critical. For example, during the pre-operative period understanding through direct discussion with a patient how their previous traumatic experiences might inform their perioperative experience and the need for a personalized pain management plan. Increased collaboration with patients, experts in Addiction Medicine and Psychiatry, patient advocacy groups, primary care providers, and other care partners is also key.
In addition, with advances in treatment and the growing importance of socio-demographic factors, educational assets for anesthesiologists should be updated with content specific to addiction. Finally, the authors urge anesthesiologists to start viewing their role as one beyond pain management. Greater involvement in harm reduction interventions and surgical rehabilitation are two suggested areas.
The continuing evolution of both our understanding of addiction and substance abuse, and SUD management make high-quality studies and randomized controlled trials challenging. Objectives of these new approaches are to prevent relapse, reduce harm, minimize pain, and improve the overall well-being of people with SUDs. Goel and Lamba are proposing a system where relevant decision makers (patients, substance use experts) and appropriate stakeholders are involved in the policies and decisions that affect persons with SUDs.
More information: Akash Goel et al, Nothing About Us Without Us: A Solution to Iatrogenic Perioperative Morbidity and Mortality in People Who Use Drugs, Anesthesia & Analgesia (2023). DOI: 10.1213/ANE.0000000000006571
Read the Substance Use Disorders issue of Anesthesia & Analgesia.