This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
proofread
Count of neurosurgeon density reflects global unmet needs
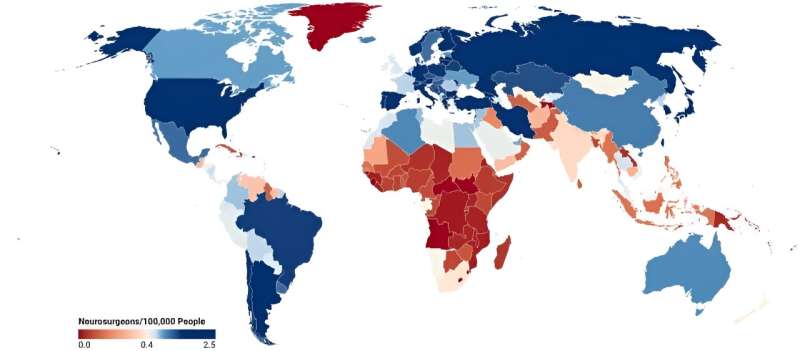
How many neurosurgeons are needed worldwide? Recent reports have suggested that a neurosurgeon ratio of approximately 1 neurosurgeon per 65,000 individuals may not be adequate.
Investigators from Harvard Medical School attempted to systematically provide the most accurate count of neurosurgeon density around the world, as well the number in each country. Using data collected from 99.5% of all countries and 96.2% of all additional territories, states, and disputed regions, the authors report that there are approximately 72,967 neurosurgeons globally, representing a pooled density of 0.93 neurosurgeons per 100,000 individuals, and a median national density of 0.44 neurosurgeons per 100,000 individuals.
The study detailing these findings was published today in the Journal of Neurosurgery
The authors used contacts with national and regional neurosurgery societies, their own personal contacts, bibliometric and Google searches, and World Bank and United Nations data to obtain perhaps the most accurate count of global neurosurgeon density to date.
There were wide disparities in the neurosurgery workforce and access to resources in different WHO regions and World Bank income categories. The African region, with 0.11 neurosurgeons per 100,000 individuals, and the Southeast Asia region, with 0.34 per 100,000 individuals, had the lowest neurosurgeon density, while the Western Pacific region (WPR) had the highest density, with 1.58 per 100,000 individuals.
The authors found that there were 29 countries, 14 territories, and one independent state with no neurosurgeons at all, representing almost 36 million individuals without access to a neurosurgeon. Among these 29 countries, 21 were low- and middle-income countries (LMICs; 72.4%), and most were located in the WPR (n = 10, 34.5%) or African region (n = 9, 31.0%).
The greatest growth in the number of neurosurgeons from 2016 to 2022 was in the Southeast Asia region (33.0% per year), while the slowest growth was in the African region (2.0% per year); 15 countries in the African region had a decrease in their neurosurgery densities, and seven of these 15 countries were in West Africa. Some of the strongest predictors of annual relative growth in neurosurgery density included the presence of a national neurosurgery society, development aid, and national gross domestic product.
"We were excited to find that the neurosurgery workforce is growing worldwide, but the growth in LMICs has been disproportionately slow," said Dr. Saksham Gupta, the lead author of the study. "The number of neurosurgeons in many LMICs remains insufficient to manage their countries' needs, and neurosurgeons in LMICs have fewer resources to provide subspecialized care. These imbalances will negatively affect population health in LMICs and could contribute to burnout among already overworked LMIC neurosurgeons."
In a related companion article, the authors also attempted to determine the global density of neurosurgeon trainees. They estimated there were 1,261 training programs with 10,546 neurosurgery trainees worldwide. The Southeast Asia (0.04 per 100,000 people) and African (0.05 per 100,000 people) regions had the lowest pooled trainee density, and there were no training programs in 22.4% of high-income countries (HICs) and in 35.2% of LMICs.
Surveys of African young neurosurgeons and trainees highlighted some of the educational limitations that most trainees face, which included low exposure to educational conferences, the inability to attend national and international research conferences, and low access to cadaver laboratories.
Regarding solutions to correct these imbalances, Gupta stated, "Collaboration between LMICs and HICs as well as between LMICs themselves is key and will help new perspectives flourish and best practices spread. Furthermore, there have been several impressive educational efforts, including but certainly not limited to Dr. Rutka's work with the Ukraine Pediatric Fellowship Program, Dr. Baticulon's work in the Philippines, the World Federation of Neurosurgical Societies (WFNS)—sponsored training center in Rabat, and numerous Foundation for International Education in Neurological Surgery courses and partnerships.
"Education is the bedrock of neurosurgery, and we should continue supporting existing educational tools (such as cadaver laboratories, weekend courses, year-long fellowships) while promoting emerging teaching modalities (webinars, high-fidelity dissection models, and open-access operative videos)."
More information:
Saksham Gupta et al, Mapping the global neurosurgery workforce. Part 1: Consultant neurosurgeon density, Journal of Neurosurgery (2024). DOI: 10.3171/2023.9.JNS231615.
thejns.org/view/journals/j-neu … 2023.9.JNS231615.xml
Saksham Gupta et al, Mapping the global neurosurgery workforce. Part 2: Trainee density, Journal of Neurosurgery (2024). DOI: 10.3171/2023.9.JNS231616. thejns.org/view/journals/j-neu … 2023.9.JNS231616.xml