This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
proofread
New technique detects novel biomarkers for kidney diseases with nephrotic syndrome
A study, presented at the 61st ERA Congress, has uncovered a significant breakthrough in the diagnosis and monitoring of kidney diseases associated with nephrotic syndrome. The study is also published in the New England Journal of Medicine.
Using a hybrid technique, researchers identified anti-nephrin autoantibodies as a reliable biomarker for tracking disease progression, opening new avenues for personalized treatment approaches.
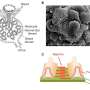
Nephrotic syndrome, characterized by elevated protein levels in the urine, is linked to kidney diseases such as minimal change disease (MCD), primary focal segmental glomerulosclerosis (FSGS), and membranous nephropathy (MN). The primary cause behind nephrotic syndrome is damage to podocytes, the cells responsible for filtering the kidneys, which allows protein to leak into the urine.
Children diagnosed with MCD or FSGS often receive a diagnosis of idiopathic nephrotic syndrome (INS), where the cause of the nephrotic syndrome is unknown. This is frequently because children with high protein levels in their urine rarely undergo a kidney biopsy, which is how the cause is typically determined.
Traditionally, diagnosing these conditions has posed challenges due to overlapping histological features and hesitancy to conduct invasive kidney biopsies, particularly in children. While anti-nephrin autoantibodies have been observed in certain patients with MCD and FSGS, their precise role in the advancement of these diseases is not fully understood.
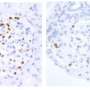
The study, conducted across Europe and the U.S., introduced a novel approach combining immunoprecipitation with enzyme-linked immunosorbent assay (ELISA) to reliably detect anti-nephrin autoantibodies.
The findings revealed that anti-nephrin autoantibodies were prevalent in 69% of adults with MCD and 90% of children with INS who had not been treated with immunosuppressive drugs. Importantly, the levels of these autoantibodies correlated with disease activity, suggesting their potential as a biomarker for monitoring disease progression. The antibodies were also rarely seen in the other diseases under examination.
To further investigate the impact of nephrin immunization on kidney function and disease, researchers administered laboratory-made nephrin protein to mice, creating a condition akin to MCD in the mice. Immunization led to the phosphorylation of nephrin and notable alterations in cell structure, indicating the involvement of antibodies targeting nephrin in podocyte malfunction and nephrotic syndrome.
Remarkably, unlike other models necessitating multiple immunizations, this model induced swift disease manifestation with a single immunization, even at low antibody concentrations.
Dr. Nicola M. Tomas, co-lead author of the study, commented, "The identification of anti-nephrin autoantibodies as a reliable biomarker, coupled with our hybrid immunoprecipitation technique, enhances our diagnostic capabilities and opens new avenues for closely monitoring disease progression in kidney disorders with nephrotic syndrome."
Professor Tobias B. Huber, lead author of the study, furthered, "By providing insights into underlying mechanisms, these findings lay the groundwork for personalized interventions and pave the way for a new era of precision medicine for these complex conditions."
More information: Tobias B. Huber et al, Autoantibodies Targeting Nephrin in Podocytopathies, New England Journal of Medicine (2024).