This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
peer-reviewed publication
trusted source
proofread
MRI and AI could significantly reduce pediatric brain tumor diagnosis time

Children with the most common malignant form of brain cancer could see diagnostic wait times reduced thanks to new research that trialed a new, quicker and less invasive way of determining which type of tumor they have.
The study, published in eBioMedicine, was conducted by a team of researchers led by the University of Birmingham and Newcastle University, with Birmingham Children's Hospital as the lead clinical center.
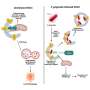
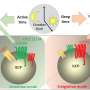
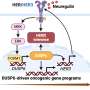
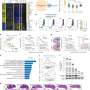
The collaborative team identified how the four different groups of medulloblastoma, a malignant children's brain tumor, had a specific profile based on their individual metabolism. Taking cell samples from 86 tumors, a laboratory test was used to accurately identify metabolic markers including chemicals specific to the different tumor groups.
The study also validated previous research that found that glutamate, a metabolite present across all of the tumor cells, is linked closely with tumor prognosis.
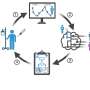
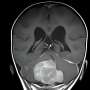
Significantly, the research could pave the way for using MRI scanning combined with machine learning to assess medulloblastomas for their 'signature' metabolic profiles without the need for invasive biopsy and could rapidly reduce the current 3-4 week wait from presentation to full diagnosis.
Andrew Peet, Emeritus Professor of Clinical Pediatric Oncology at the University of Birmingham and an Honorary Consultant at Birmingham Women's and Children's NHS Foundation Trust, who is lead author of the study said, "Time is so important in cancer diagnosis so our findings on different types of medulloblastoma having a detectable signature metabolism could be game changing for quickly diagnosing, and then offering the best possible treatment for children."
Professor Steve Clifford, Chair of Molecular Pediatric Oncology at the Newcastle University Center for Cancer, who jointly led the study said, "Providing a rapid diagnosis using innovative scanning and AI (artificial intelligence) techniques, has the potential to revolutionize patient management, allowing early non-invasive diagnosis, tailoring of treatment decisions and reducing the period of uncertainty for patients and parents while awaiting a full diagnosis.
"Further, our biological findings provide critical new insights into the metabolism underpinning these tumors, and the potential to exploit these therapeutically."
The latest findings could be game changing for children like Jack Bourne, aged six, from Birmingham who was diagnosed with medulloblastoma in March 2023.
Jack's dad Tom said, "We've been through 13 months of treatment but six weeks of that was just waiting to find out what type of tumor he had. We were so scared."
Within weeks of starting school, Jack had started experiencing sickness and headaches which doctors put down to possible separation anxiety or vertigo. But when parents Tom and Tom and Suzanna noticed that he was struggling to walk, they sought a second opinion and Jack was referred to Birmingham Children's Hospital the same day.
"When they told me the results of the MRI scan, I didn't know what to feel," said Tom. "As we were trying to digest everything, they were asking us to sign consent forms because they wanted to operate first thing the next morning. You're reading these forms and all you see is—he might not make it out alive. It's heartbreaking, it really is."
Jack pulled through the 10-hour operation to remove the tumor, but it would take more than four weeks for doctors to figure out what specific type of medulloblastoma he had in order to effectively treat it.
"The research that's going into diagnosing tumors is really important," said Tom. "In Jack's case there was quite a delay while they sent his tumor to Great Ormond Street to be analyzed. During that time Jack was given some chemo just to start things off because they just wanted to do something rather than just wait. But all you want is for your child to be given the best possible treatment right from the start."
Improving outcomes for every child
Christiana Ogunbote, head of research at Children with Cancer UK said, "We are incredibly proud to help fund this innovative medulloblastoma research and are excited to see how it could change the experiences of children diagnosed with this disease and their families.
"Discovering new ways to improve outcomes for children with cancer is at the heart of what we are trying to achieve. Through continued and sustained investments in research we look forward to a day where every child can survive their cancer diagnosis."
Dr. Laura Danielson, children's and young people's research lead at Cancer Research UK, said, "Developing quicker, less invasive ways to accurately diagnose the different types of medulloblastoma, the most common malignant brain tumor in children, is a crucial step in improving outcomes for young patients.
"This important study has identified a new way to distinguish between the four subgroups of medulloblastoma. This discovery paves the way for the development of simple imaging tests that could quickly and accurately diagnose the different types of medulloblastoma.
"This kind of discovery research is important to drive new and improved ways to better detect and treat cancers affecting children and young people."
More information: Sarah Kohe et al, Metabolite profiles of medulloblastoma for rapid and non-invasive detection of molecular disease groups, eBioMedicine (2024). DOI: 10.1016/j.ebiom.2023.104958