This article has been reviewed according to Science X's editorial process and policies. Editors have highlighted the following attributes while ensuring the content's credibility:
fact-checked
trusted source
proofread
Precision medicine for sepsis in children within reach
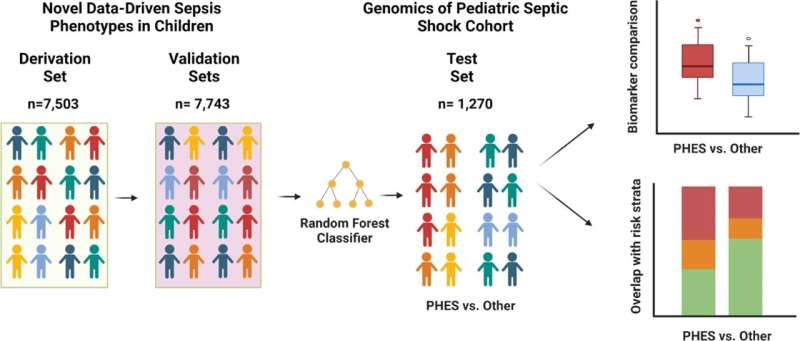
Sepsis—the leading cause of mortality in children around the world—can present with a wide range of signs and symptoms, making a one-size-fits-all treatment strategy ineffective. Pursuing a precision medicine approach for pediatric sepsis, researchers used artificial intelligence to analyze a large set of clinical data and find a distinct group of patients who might respond better to targeted treatments.
These children share clinical characteristics described as PHES, or persistent hypoxemia (abnormally low oxygen levels in the blood), encephalopathy (brain function disturbance) and shock, which is a highly lethal pattern within sepsis presentations. A recent study validated this pattern and discovered that PHES overlaps with biomarkers that indicate excessive levels of inflammation and endothelial activity (which works in tandem with an overactive immune response). Findings were published in the journal Pediatric Critical Care Medicine.
"The association we found between PHES and a set of biomarkers suggests that this group of children with sepsis could benefit from targeted treatment, such as corticosteroids, for example," said senior author L. Nelson Sanchez-Pinto, MD, critical care physician as well as Warren and Eloise Batts Research Scholar at Ann & Robert H. Lurie Children's Hospital of Chicago, and Associate Professor of Pediatrics and Preventive Medicine at Northwestern University Feinberg School of Medicine. "In sepsis care, physicians need to make quick treatment decisions and our study shows that they can base these decisions on a specific pattern within routinely collected clinical data. We are much closer now to precision medicine for sepsis."
Dr. Sanchez-Pinto explains that clinical trials are still needed to test various targeted treatments for children with PHES. He expects that within the next five years there will be enough research data to change clinical practice and make it more consistent.
"Our findings also allow more targeted research into treatments for sepsis," he said. "Studies might show that a treatment is ineffective for children with sepsis overall, but that same treatment could be studied in children with PHES and prove to be life-saving for this distinct group of patients."
More information: Mihir R. Atreya et al, Biomarker Assessment of a High-Risk, Data-Driven Pediatric Sepsis Phenotype Characterized by Persistent Hypoxemia, Encephalopathy, and Shock, Pediatric Critical Care Medicine (2024). DOI: 10.1097/PCC.0000000000003499