Autism may involve disordered white matter in the brain
It's still unclear what's different in the brains of people with autism spectrum disorders (ASDs), but evidence from genetic and cell studies points to abnormalities in how brain cells (neurons) connect to each other. A study at Children's Hospital Boston now provides visual evidence associating autism with a disorganized structure of brain connections, as well as defects in myelin -- the fatty, insulating coating that helps nerve fibers conduct signals and that makes up the brain's white matter.
Researchers led by Mustafa Sahin, MD, PhD, of the Department of Neurology, Simon Warfield, PhD, director of the Computational Radiology Laboratory, and first author Jurriaan Peters, MD, of both departments at Children's, used advanced magnetic resonance imaging (MRI) to image the brains of 40 patients (infants to age 25) with tuberous sclerosis complex and 29 age-matched, healthy controls. Tuberous sclerosis is a rare genetic condition often associated with cognitive and behavioral deficits, including ASDs about 50 percent of the time.
"Patients with tuberous sclerosis can be diagnosed at birth or potentially before birth, because of cardiac tumors that are visible on ultrasound, giving us the opportunity to understand the circuitry of the brain at an early age," explains Sahin. "Our ultimate goal is to use imaging in infancy to find which tuberous sclerosis patients are at high risk for autism so we can intervene early. This may have implications for autism in patients without tuberous sclerosis as well."
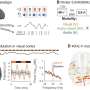
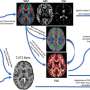
The team used a relatively new MRI technique called Diffusion Tensor Imaging to trace the pathways of nerve fibers by measuring the diffusion of water in the brain. In the January issue of the journal Academic Radiology, they report findings in the corpus callosum, the brain's largest white-matter structure that acts as a highway transferring signals between the left and right cerebral hemispheres.
Of the 40 patients with tuberous sclerosis, 24 had clinically significant developmental delays or intellectual disability, and 12 had ASDs. ASDs were diagnosed clinically by a pediatric neurologist, and, in most cases, by the Autism Diagnostic Observation Schedule (ADOS).
In general, compared with controls, patients with tuberous sclerosis had higher radial diffusivity values, a measure of water diffusion out of (perpendicular to) the nerve fibers (axons). Radial diffusivity is an indirect measure of how well insulated the axons are: Having higher radial diffusivity means axons are poorly insulated with myelin, suggesting abnormalities in the white matter (which is partly made up of myelin.
Patients with both tuberous sclerosis and ASDs not only had increased radial diffusivity -- compared with both non-ASD patients and controls -- but they also had clearly disorganized axon pathways.
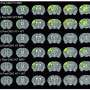
As shown in the images, axons in the control subjects followed well-defined directions in organized bundles (left panels), while the ASD patients' axons (right panels) tended not to orient together in common directions (referred to in the paper as having lower fractional anisotropy). Tuberous sclerosis patients without ASDs (middle panels) showed only slight disorganization compared to controls.
"This study shows that we can use diffusion tensor imaging to differentiate tuberous patients with autism from those without autism," says Sahin.
"Our advances in imaging and in image analysis are enabling us to identify and quantitatively characterize alterations in brain development that are not readily visible in conventional imaging,'' adds Warfield.
The findings add to previous human imaging studies by Sahin and Warfield showing similar differences in the brain's visual cortex, and are consistent with brain MRIs in older, high-functioning individuals with ASDs, showing abnormalities in connectivity in the corpus callosum and in areas of brain involved in language and social skills.
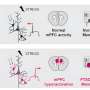
The findings are also consistent with studies in Sahin's lab using mouse models of tuberous sclerosis. The neurons in these mice grew multiple axons (normal neurons grow just one), causing too many connections being made, and axons originating in the retina failed to land in the right places in the brain and did not respond to navigation cues.
Additional studies showed that the axons in these mice had less myelination, identified the biochemical pathway causing these defects, known as the mTOR pathway, and showed that the pathway and the myelination defects could be reversed in mice with the mTOR-inhibiting drug rapamycin.
Armed with these data, Sahin has launched a Phase II clinical trial of a rapamycin-like drug called Afinitor® (everolimus; formerly RAD001), sponsored by Novartis, the Tuberous Sclerosis Alliance and Autism Speaks. The trial will enroll 50 patients with TSC to test whether Afinitor improves neurocognition, autism, seizures and sleep disorders. "Specifically modulating neurocognition with a small molecule is only starting to be done," says Sahin. (For more on this trend, see this related blog post.)
"Ultimately, imaging will play a crucial role in identifying who may benefit from treatment, and in seeing the changes in the brain in response to treatment," says Warfield.