Stanford researcher to expand DNA database by adding Latin Americans

(Medical Xpress) -- Genetic mapping has led scientists to a better understanding of human disease and how to fight ailments like diabetes, mental illness and cancer.
But the information they have to work with is limited, drawing mostly from the DNA of people with European bloodlines. When it comes to figuring out how genetic disorders affect groups who don't share that ancestry or have only trace amounts of it in their family histories, researchers are often at a loss.
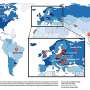
Andres Moreno is changing that. Thanks to the $100,000 he is receiving as this year's recipient of the George Rosenkranz Prize for Health Care Research in Developing Countries, the Stanford researcher will analyze the DNA of indigenous groups and cosmopolitan populations living in Mexico, South America and the Caribbean.
The data he gathers will lay the groundwork for scientists interested in knowing how genetic diseases take hold and manifest themselves among Latin Americans – one of the most underrepresented populations in the field of genetics.
"We can't start talking about how to deliver personalized medicine in Latin America because we still have much to learn about their genetic makeup at the population level," said Moreno, a research associate in the Department of Genetics at the School of Medicine.
"We need to draw the genetic map that will allow us to better understand the genetic basis of multiple conditions that lead to major health problems in Latin America," he said.
Scientists have found numerous genetic variants linked to complex traits among people with European backgrounds, and that connection has allowed doctors to better treat and prevent diseases in that group.
But without a rich database built on the DNA of people whose family trees are rooted in Latin America, researchers have yet to find the genetic key to explain why descendants of the region's indigenous populations are predisposed to particular conditions.
Obesity, for example, is more prevalent in Mexico than in other parts of the world, Moreno said.
"We need to find population-specific gene variants that don't exist anywhere else but locally," he said. "Then we can maybe find the gene behind obesity there."
Other conditions may be addressed by studying locally adapted populations, such as those living at high altitude in the Andes, where pregnant women have a fivefold higher rate of maternal hypertension than the native population.
"We are trying to identify the genetic variants underlying the mechanisms for this protection, which may help to design preventive and therapeutic measures worldwide," Moreno said.
Stanford's Center for Health Policy, a center of the university's Freeman Spogli Institute for International Studies, administers the Rosenkranz award that will fund Moreno's work. The prize was created in 2007 to foster the research of a young Stanford scholar committed to improving health care in developing countries and reducing health disparities across the globe.
The first recipient was Eran Bendavid, an assistant professor of medicine and an associate of the Center for Health Policy.
"We believe Andres' work will deepen our understanding of the genetics of disease across populations, and we are delighted to recognize his important scientific contributions," said Douglas Owens, director of the Center for Health Policy.
The Rosenkranz Prize was established by the friends and family of Dr. George Rosenkranz, the scientist who helped first synthesize cortisone in Mexico in 1951. Rosenkranz, who lives in Menlo Park, Calif., also synthesized the active ingredient for the first oral birth control and served as a chief executive officer of Syntex, a Mexican pharmaceutical company.
In addition to Owens – who is the Henry J. Kaiser, Jr. Professor in the School of Medicine and a senior fellow at the Freeman Spogli Institute – members of the award selection committee included Donald Kennedy, president emeritus of Stanford; Rosamond Naylor, the William Wrigley Senior Fellow at FSI and the Stanford Woods Institute for the Environment; Paul Yock, the Martha Meier Weiland Professor in the School of Medicine and professor of bioengineering; and Michele Barry, the medical school's senior associate dean for global health and director of the Center for Innovation in Global Health.