Universal influenza vaccine potentially in sight
The fall ritual of getting an annual influenza shot could join castor oil on the list of bygone remedies within a decade, some scientists say. And as that tradition fades away, so too will our fears of the virus mutating into a global pandemic.
To many, the concept of a world free from the coughs and fevers brought on by influenza sounds improbable—impossible, even.
If you listen to media reports, influenza seems to be gaining strength. In 2009, swine flu reached pandemic levels in the human population, while avian flu killed millions of birds worldwide. In 2012, a new strain of swine flu sickened children attending a state fair. And early this year, the virus rose for two consecutive weeks to epidemic levels, with 7.3% of deaths attributed to influenza or pneumonia.
By anyone's scorekeeping, influenza is winning.
Yet technology and dogged determination have given scientists a fighting chance and renewed optimism. During research over the last several years at the Advanced Photon Source at Argonne, two teams of scientists closed on what they suspect is the virus's Achilles' heel.
"There is a lot of hope that a universal flu vaccine is not as far off as we used to think," said Damian Ekiert, a research scientist at the University of California, San Francisco.
Insight into how the virus works—and where it is collectively weakest—came out of a mix of research that combines computer modeling of the virus and X-ray crystallography to unravel the structure of individual proteins in the virus. These proteins often contain thousands of atoms tightly interwoven in a seemingly random pattern, like the world's most challenging knot. To identify a protein that could serve as a target for new pharmaceuticals, scientists have to puzzle out how the atoms and their bonds fit together and identify vulnerable sites where the immune system could target.
Our immune system fights viral infections by creating antibodies that attach to proteins on the surface of the virus and block its ability to enter a healthy cell. However, influenza has many subtypes, or strains, and the virus mutates quickly, so researchers have to predict which strains are most likely to spread that year and create a flu shot for those viruses.
Decades of research have revealed that the most effective antibodies target a protein called hemagglutinin. Hemagglutinins are the molecules on the flu virus that let it invade the cells of respiratory passages. These flower bouquet-shaped proteins are common targets for influenza vaccinations, which aim to block the hemagglutinin from latching onto healthy cells. Each strain of influenza has a slightly different hemagglutinin. Current vaccinations work on just a small subset of strains—so if the virus mutates, the vaccination fails.
In order to overcome this variability among influenza virus strains, a team of researchers at the Dutch biotechnology company Crucell set out to identify antibodies that worked against several strains.

Ekiert, then a graduate student in Ian Wilson's laboratory at The Scripps Research Institute, got the task of identifying which spot on hemagglutinin the antibodies were targeting.
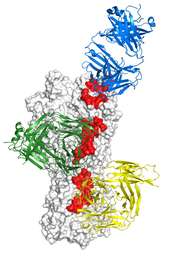
Using the high-energy X-ray beam at the Advanced Photon Source, Ekiert determined the structure of several antibodies bound to the hemagglutinin protein. Remarkably, the structures revealed that while the head of the protein changed with each substrain of influenza, the antibodies bound to a region on the stem that remains essentially the same in all strains and subtypes.
It was a discovery that has changed the direction of influenza research. Now several teams of scientists are starting to find antibodies that neutralize an entire group—or even all the flu strains—instead of focusing on a single seasonal form.
The early results are good. The new attack strategies could very well shift the balance of power to humanity and away from a virus that, in its 1918 incarnation, killed millions of people around the world.
One of the tools that gave Ekiert the upper hand against this virus, which others have studied for decades, was the invention of techniques such as a micron-sized X-ray beam and automated computerized rastering at an Advanced Photon Source beamline called the General Medical Sciences and Cancer Institutes Structural Biology Facility. That unique tool allows scientists to quickly scan the landscape of a biological sample and hone in on a smaller area for scrutiny than ever before. It's as if on Ekiert's mission to scout out the best way that the immune system can attack the virus, he was given super binoculars. Ekiert admitted that this gave him an edge.
"Tools developed here were crucial for the collection of high-quality diffraction data," Ekiert said. "Several of the structures would have been difficult or perhaps impossible to obtain at many other beamlines."
The micro-X-ray beam allowed him to see how the antibodies bind to the hemagglutinin protein—and thus how they are so effective at neutralizing the virus.
Three of the most promising advances stem from this APS research.
Industrial research partners at Crucell Vaccine Institute have been developing these antibodies into new therapies for influenza, including human clinical trials.
A research team led by Wilson has now found multiple human monoclonal antibodies that bind to the portions of the hemagglutinin that protect against infection from several influenza strains.
Another very promising area of research led by University of Washington professor David Baker uses computer modeling to design proteins from scratch that will bind to the virus to keep it from entering a healthy cell. Baker has successfully made proteins that bind to all types of a particular group of hemagglutinins, which includes the strains H1, or swine flu; H5, or avian flu; and H2, or Asian flu. Baker plans to create a database of proteins that would fight potential mutations of various influenza strains. This would save scientists valuable time by not having to grow protein samples, sort through hundreds of potential drug proteins, and then find a live virus to test them against. Instead, these designed proteins could be tested with advanced computer modeling and stored in a database accessible to drug manufacturers.
A universal vaccine would change the way influenza shots are manufactured. No longer would companies have to wait for the first wave on infection to start designing an antibody. People would be protected from childhood on, ideally with one shot and one or two boosters in adulthood. Influenza would become like polio or whooping cough or measles: a serial killer rendered powerless by the use of preventative medicine.
Just like ending any war, victory over influenza would send ripples through national economies. Each year in the United States, about 10% of the population gets sick from the influenza virus; 36,000 die. Hospitalization related to influenza costs the U.S. about $10 billion annually.
Ekiert thinks advances in high-energy X-ray technology might accelerate studies that could reveal similar commonalities in other stubborn viruses and potentially unlock new treatments.
"You could imagine trying to take this approach to target any pathogen that mutates or has been difficult to design a vaccine for, such as tuberculosis, malaria, or HIV," he says.