Study may explain link between antibiotic use in infants and asthma

(Medical Xpress)—Children who receive antibiotics before their first birthday might be at a slightly increased risk of developing asthma. However, new research by The University of Manchester suggests that it is impaired viral immunity and genetic variants on a region of chromosome 17 that increase the risk of both antibiotic use in early life and later asthma rather than the antibiotics themselves, as previously thought.
Importantly, the study, which was funded by the Medical Research Council and J P Moulton Charitable Foundation did not find a link between early antibiotic prescription and the development of allergic reactions.
The findings, reported in The Lancet Respiratory Medicine today (15 May), contradict the prevailing theory that early antibiotic exposure, via changes in gut flora, alters the development of a child's immune system, increasing susceptibility to allergic asthma later on.
In children, antibiotics are routinely used to treat respiratory infections, ear infections, and bronchitis, and several studies have reported a link between the use of antibiotics during early childhood and the subsequent development of asthma. However, systematic reviews have reported conflicting results and called for additional longitudinal studies to provide definitive answers.
In this study, UK researchers examined data from the Manchester Asthma and Allergy Study (MAAS) which has followed over 1000 children from birth to 11 years.
Information on antibiotic prescription, wheeze and asthma exacerbations were taken from medical records. Skin reaction tests that show whether a child is hypersensitive to allergens were done at ages 3, 5, 8, and 11 years.
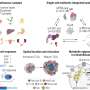
At age 11, blood was collected from children who had received at least one course of antibiotics or no antibiotics in the first year of life to compare their immune-system cell response to viruses (rhinovirus; the virus responsible for the common cold, and respiratory syncytial virus; RSV) and bacteria (Haemophilus influenzae and Streptococcus pneumoniae). Genetic testing was also done to look at the links between common genetic variations on chromosome 17, known as 17q21, and antibiotic prescription.
The study's findings are believed to be the first to show that children with wheezing who were treated with an antibiotic in the first year of life were more than twice as likely as untreated children to experience severe wheeze or asthma exacerbations and be hospitalised for asthma.
Similarly, these children also showed significantly lower induction of cytokines, which are the bodies' key defence against virus infections such as the common cold. However, no differences were noted in antibacterial responses.
The researchers also identified two genes in the 17q21 region that were associated with an increased risk of early life antibiotic prescription.
Lead author Professor Adnan Custovic, from the Institute of Inflammation and Repair based at The University of Manchester, said: "We speculate that hidden factors which increase the likelihood of both antibiotic prescription in early life and subsequent asthma are an increased susceptibility to viral infections due to impaired antiviral immunity and genetic variants on 17q21.
"However, further studies will be needed to confirm that the impaired immunity was present at the time of the early childhood respiratory symptoms and predated antibiotic prescribing rather than as a consequence of the antibiotics."
More information: The complete study is available online: press.thelancet.com/asthmaantibiotics.pdf