Choosing one drug over another to treat blindness could save Medicare billions
If all eye doctors prescribed the less expensive of two drugs to treat two common eye diseases of older adults, taxpayer-funded Medicare plans could save $18 billion over a 10-year period, say researchers at the University of Michigan.
Further, patients with the wet form of macular degeneration or who have diabetic macular edema could keep $4.6 billion in co-pays in their wallets, and the rest of the U.S. health care system could save $29 billion in private insurance payments and other costs, according to the team led by David Hutton, assistant professor of health management and policy at the U-M School of Public Health.
The reason for the dramatic savings: bevacizumab (marketed under the name Avastin) costs $55 per treatment and ranibizumab (trade name Lucentis) runs $2,023 for each dose—nearly 40 times more expensive. Yet, the drugs have similar efficacy in treating these conditions, and both have fairly comparable side effect and safety profiles when used to treat eye disease, the researchers say.
"As the Medicare-eligible population continues to grow, identifying savings while maintaining quality patient care is increasingly important," Hutton said. "People don't like to think there are tradeoffs between health and costs but we certainly do need to think about cost when health care is 18 percent of the GDP and growing."
More than 2 million patients—most over the age of 65—currently have these eye diseases, and it is estimated that by 2020 nearly 3 million people will experience visual impairment from age-related macular degeneration.
The team's report, featured in the June issue of Health Affairs, comes on the heels of a national debate over data released in April 2014 by the Centers for Medicare and Medicaid Services, showing that 17,000 ophthalmologists collectively received $5.6 billion in Medicare payments in 2012. The report showed that ophthalmologists had some of the highest payment totals among physicians, and the largest percentage of the reimbursements to these specialists was to cover the cost of ranibizumab.
In 2010, federal spending on the two drugs totaled $2 billion, approximately one-sixth of the entire budget for Medicare Part B, which covers the cost of doctor visits and other nonhospital services. Both drugs are injected into the eye by ophthalmologists during an office visit, so they are covered by Part B instead of the Medicare prescription drug benefit Part D.
To calculate the savings, the researchers used sophisticated modeling methods to predict population-level costs for the decade spanning 2010-20 based on current use of the two drugs.
So why is one drug so much more costly?
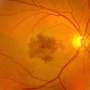
Bevacizumab originally was created as a cancer-fighting drug, given in much higher doses to slow the development of blood vessels, thereby inhibiting the growth of tumors. In diabetic macular edema and one form of macular degeneration, it is the abnormal growth of blood vessels in the retina that causes blindness. Used in the eye, the medication targets the bleeding and swelling that occurs in the retina and shrinks the blood vessels, says study co-author Dr. Joshua Stein, assistant professor of Ophthalmology and Visual Sciences at the Medical School and U-M Kellogg Eye Center.
For a number of years physicians have used bevacizumab to treat these eye conditions off label, meaning prescribed for a use other than the one originally intended. In its full dose for cancer treatment (at 150 times the concentration of the ocular injections), the drug is more expensive, but the cost goes down when reduced to smaller doses for the eye.
The same drug company that manufactured bevacizumab created ranibizumab, which was approved by the FDA as a drug targeted at these eye diseases. In doing so, the company attached the higher price to the new drug.
Both are in a class known as biologic drugs, which are large complex molecules manufactured within living cells and are costly to develop and manufacture.
"These relatively new drugs, the first available beginning in the mid-2000s, have revolutionized treatment for these eye diseases," Stein said. "Not only have they prevented vision from getting worse for many patients, a number of patients have seen an improvement in their vision."
Today, about two-thirds of eye doctors prescribe bevacizumab. Because it was tested and approved by the FDA for cancer treatment, however, the original safety data addresses side effects at the higher dose. In some patients, these include stroke and heart attack. But data at the lower dose used to treat patients with ocular conditions is limited, Stein says, perhaps explaining some ophthalmologists reluctance to use the drug.
"In two large clinical trials that have been done on use in eye disease, the data did not show a difference in rates of serious side effects, but those studies didn't have enough power to fully address safety," he said.
The researchers want their analysis to capture the attention of health policymakers.
"I hope that this study raises awareness of the rest of the medical community, sheds light on the issue of the cost of biologic drugs, and brings attention to how long it takes to get biosimilars (generic versions) of these drugs approved," Hutton said.
More information: content.healthaffairs.org/cont … nt/33/6/931.abstract