New study throws into question long-held belief about depression
New evidence puts into doubt the long-standing belief that a deficiency in serotonin—a chemical messenger in the brain—plays a central role in depression. In the journal ACS Chemical Neuroscience, scientists report that mice lacking the ability to make serotonin in their brains (and thus should have been "depressed" by conventional wisdom) did not show depression-like symptoms.
Donald Kuhn and colleagues at the John D. Dingell VA Medical Center and Wayne State University School of Medicine note that depression poses a major public health problem. More than 350 million people suffer from it, according to the World Health Organization, and it is the leading cause of disability across the globe. In the late 1980s, the now well-known antidepressant Prozac was introduced. The drug works mainly by increasing the amounts of one substance in the brain—serotonin. So scientists came to believe that boosting levels of the signaling molecule was the key to solving depression. Based on this idea, many other drugs to treat the condition entered the picture. But now researchers know that 60 to 70 percent of these patients continue to feel depressed, even while taking the drugs. Kuhn's team set out to study what role, if any, serotonin played in the condition.
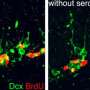
To do this, they developed "knockout" mice that lacked the ability to produce serotonin in their brains. The scientists ran a battery of behavioral tests.
Interestingly, the mice were compulsive and extremely aggressive, but didn't show signs of depression-like symptoms. Another surprising finding is that when put under stress, the knockout mice behaved in the same way most of the normal mice did. Also, a subset of the knockout mice responded therapeutically to antidepressant medications in a similar manner to the normal mice. These findings further suggest that serotonin is not a major player in the condition, and different factors must be involved. These results could dramatically alter how the search for new antidepressants moves forward in the future, the researchers conclude.
More information: "Mice Genetically Depleted of Brain Serotonin Do Not display a Depression-like Behavioral Phenotype" ACS Chem. Neurosci., Article ASAP. DOI: 10.1021/cn500096g
Abstract
Reductions in function within the serotonin (5HT) neuronal system have long been proposed as etiological factors in depression. Selective serotonin reuptake inhibitors (SSRIs) are the most common treatment for depression, and their therapeutic effect is generally attributed to their ability to increase the synaptic levels of 5HT. Tryptophan hydroxylase 2 (TPH2) is the initial and rate-limiting enzyme in the biosynthetic pathway of 5HT in the CNS, and losses in its catalytic activity lead to reductions in 5HT production and release. The time differential between the onset of 5HT reuptake inhibition by SSRIs (minutes) and onset of their antidepressant efficacy (weeks to months), when considered with their overall poor therapeutic effectiveness, has cast some doubt on the role of 5HT in depression. Mice lacking the gene for TPH2 are genetically depleted of brain 5HT and were tested for a depression-like behavioral phenotype using a battery of valid tests for affective-like disorders in animals. The behavior of TPH2–/– mice on the sucrose preference test, tail suspension test, and forced swim test and their responses in the unpredictable chronic mild stress and learned helplessness paradigms was the same as wild-type controls. While TPH2–/– mice as a group were not responsive to SSRIs, a subset responded to treatment with SSRIs in the same manner as wild-type controls with significant reductions in immobility time on the tail suspension test, indicative of antidepressant drug effects. The behavioral phenotype of the TPH2–/– mouse questions the role of 5HT in depression. Furthermore, the TPH2–/– mouse may serve as a useful model in the search for new medications that have therapeutic targets for depression that are outside of the 5HT neuronal system.