Paradoxical Alzheimer's finding may shed new light on memory loss
Do you remember the seventh song that played on your radio on the way to work yesterday? Most of us don’t, thanks to a normal forgetting process that is constantly “cleaning house” – culling inconsequential information from our brains. Researchers at the Buck Institute now believe that this normal memory loss is hyper-activated in Alzheimer’s disease (AD) and that this effect is key to the profound memory loss associated with the incurable neurodegenerative disorder.
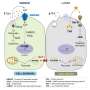
Last year, this same group of researchers found that they could completely prevent Alzheimer’s disease in mice genetically engineered with a human Alzheimer’s gene—“Mouzheimer’s”—by blocking a single site of cleavage of one molecule, called APP for amyloid precursor protein. Normally, this site on APP is attacked by molecular scissors called caspases, but blocking that process prevented the disease.
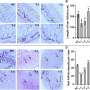
Now they have studied human brain tissue and found that, just as expected, patients suffering from AD clearly show more of this cleavage process than people of the same age who do not have the disease. However, when they extended their studies to much younger people without Alzheimer’s disease, they were astonished to find an apparent paradox: these younger people displayed as much as ten times the amount of the same cleavage event as the AD patients. The researchers now believe they know why.
The Buck Institute study implicates a biochemical “switch” associated with that cleavage of APP, causing AD brains to become stuck in the process of breaking memories, and points to AD as a syndrome affecting the plasticity or malleability of the brain. The study, due to be published in the March 7 issue of the Journal of Alzheimer’s Disease, provides new insight into a molecular event resulting in decreased brain plasticity, a central feature of AD.
“Young brains operate like Ferraris – shifting between forward and reverse, making and breaking memories with a facility that surpasses that of older brains, which are less plastic,” said Dale Bredesen, MD, Buck Institute faculty member and leader of the research group. “We believe that in aging brains, AD occurs when the ‘molecular shifting switch’ gets stuck in the reverse position, throwing the balance of making and breaking memories seriously off kilter.”
In previous research, lead author Veronica Galvan, PhD, prevented this cleavage in mice genetically engineered to develop the amyloid plaques and deposits associated with AD. These surprising mice had normal memories and showed no signs of brain shrinkage or nerve cell damage, despite the fact that their brains were loaded with the sticky A-beta plaques that are otherwise associated with Alzheimer’s disease.
“A-beta is produced throughout the brain throughout life; we believe that it is a normal regulator of the synapses, the connections between neurons,” said Galvan, who added that AD, like cancer, is a disease in which imbalanced cell signaling plays an important role.
“The fact that many people develop A-beta plaques yet show no symptoms of AD tells us that the downstream signaling of A-beta—not just A-beta itself—is critical,” said Bredesen, “and these pathways can be targeted therapeutically. Simply put, we can restore the balance.” Continuing research at the Buck Institute focuses on nerve signaling and efforts to “disconnect” the molecular mechanism that throws memory-making in the reverse direction, as well as understanding mechanisms that support brain cell connections that are crucial to the process of memory making.
Source: IOS Press