Study finds blood cells can be reprogrammed to act as embryonic stem cells
In a recent study, U.S. researchers have reprogrammed cells found in circulating blood into cells that are molecularly and functionally indistinguishable from embryonic stem cells, a revolutionary achievement that provides a readily accessible source of stem cells and an alternative to harvesting embryonic stem cells. The findings were prepublished online in Blood, the official journal of the American Society of Hematology.
Embryonic stem cells have long been coveted for their potential to treat a multitude of diseases as a result of their unique properties of nearly indefinite self-renewal and pluripotency (the ability to develop into any type of cell in the body), but their use has been the subject of political controversy.
"Our findings provide the first proof that cells from human blood can morph into stem cells," said senior study author George Q. Daley, MD, PhD, an investigator for the Howard Hughes Medical Institute at Children's Hospital, Boston. "Making pluripotent stem cells from blood, which is one of the easiest tissues to obtain, provides an easy strategy for generating patient-specific stem cells that are valuable research tools and may one day be used to treat a number of diseases."
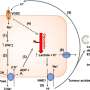
To generate induced pluripotent stem cells (dubbed iPS cells), blood was collected from a 26-year-old male donor. From the blood sample, the researchers isolated CD34+ cells, a type of stem cell that produces only blood cells, and cultured them in growth factors for six days to increase their number.
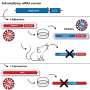
During the culture, the scientists infected the CD34+ cells with viruses carrying reprogramming factors, genes normally expressed in embryonic stem cells that can reset the blood cells to an embryonic state. Colonies of cells exhibiting physical characteristics similar to embryonic stem (ES) cells appeared about two weeks after the procedure. To determine whether these cells were also functionally similar to ES cells, the scientists analyzed the CD34+ iPS cell lines to see if they had acquired stem cell "markers," the unique combination of proteins that coat the cells' surface and distinguish them from other types of cells. Indeed, the iPS cell lines expressed the same markers as ES cells and further shared the capacity to differentiate into a variety of specialized cell types.
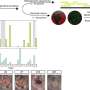
In vitro, the iPS cells readily developed into clusters of cells called embryoid bodies from which cells of virtually any type can develop. These differentiated cells expressed genes for all three embryonic germ layers (the tissues from which all other tissue types in the body develop) and also produced myeloid and granulocyte colonies (types of white blood cells).
The group confirmed that the reprogrammed cells had acquired ES cell characteristics by injecting the newly reprogrammed cells into immunodeficient mice. The cells successfully generated well-differentiated teratomas, benign masses containing all three embryonic germ layers, including respiratory, bone, and neural tissue.
"Not only has this work identified a new programmable cell type, but the cells are easy to obtain and analyze in many research laboratories and bone marrow transplantation centers around the world," said Grover C. Bagby, MD, Professor of Medicine and Molecular and Medical Genetics at Oregon Health and Science University, who is not affiliated with the study. "These findings will immediately enhance the pace of laboratory research in this field and will ultimately help to determine whether iPS cells have a therapeutic potential equivalent to that of embryonic stem cells."
Source: American Society of Hematology