Iron oxide nanoparticles becoming tools for brain tumor imaging and treatment
Tiny particles of iron oxide could become tools for simultaneous tumor imaging and treatment, because of their magnetic properties and toxic effects against brain cancer cells. In mice, researchers from Emory University School of Medicine have demonstrated how these particles can deliver antibodies to implanted brain tumors, while enhancing tumor visibility via magnetic resonance imaging (MRI).
The results are published online by the journal Cancer Research.
The lead author is Costas Hadjipanayis, assistant professor of neurosurgery at Emory University School of Medicine, director of Emory's Brain Tumor Nanotechnology Laboratory, and chief of neurosurgery service at Emory University Hospital Midtown.
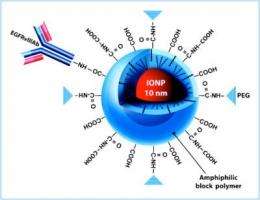
Glioblastoma multiforme (GBM), the most common and most aggressive primary brain tumor, often comes back because cancer cells infiltrate into the surrounding brain tissue and survive initial treatment. Hadjipanayis' team designed tiny iron oxide particles (10 nanometers across), coated with a polymer and bioconjugated or linked to antibodies directed against a molecule that appears on the surface of glioblastoma cells.
This molecule, a shortened and continuously active form of the epidermal growth factor receptor (EGFRvIII), drives glioblastoma cell growth and accounts for radiation and chemotherapy resistance. EGFRvIII appears in about a third of glioblastomas and is only present on tumor cells and not the normal surrounding cells in the brain.
The team showed that the particles bind to and kill human glioblastoma cells, yet do not cause any toxicity to normal human astrocytes, which comprise the majority of cells in the brain. They used a technique called convection-enhanced delivery (CED) - continuous infusion of fluid under positive pressure - to introduce the iron oxide particles into mice that had human glioblastoma cells implanted intracranially.
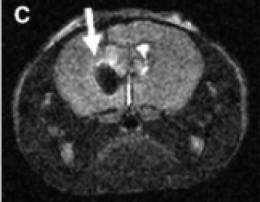
The antibody-linked particles lengthened survival of the tumor-implanted mice: their median survival was 19 days compared to 16 days for bare particles and 11 days for no particles. The particles also made the tumor visible via MRI, darkening the area of the brain where the tumor is (see accompanying image). Hui Mao, PhD associate professor of radiology, and his team of researchers, contributed MRI experiments showing the sensitive imaging qualities of the iron-oxide nanoparticles in vitro and in the mouse brain.
To heighten anti-cancer effects, the Brain Tumor Nanotechnology Laboratory is investigating the use of safe alternating magnetic fields for the generation of local hyperthermia (heating) against malignant brain tumors by magnetic nanoparticles.
Hadjipanayis and his team plan to translate the use of bioconjugated iron-oxide nanoparticles for use in canine brain tumor models at the University of Georgia College of Veterinary Medicine and into a human clinical trial for patients suffering from brain cancer.
More information: C.G. Hadjipanayis, R. Machaidze, M. Kaluzova, L. Wang, A.J. Schuette, H. Chen, X. Wu and H. Mao. EGFRvIII antibody-conjugated iron oxide nanoparticles for magnetic resonance imaging-guided convection-enhanced deliver and targeted therapy of glioblastoma. Cancer Res. 70: 6303-12 (August 1, 2010)














