Improved memory efficiency seen after aerobic exercise in fibromyalgia patients
Areas of the brain responsible for pain processing and cognitive performance changed in fibromyalgia patients who exercised following a medication holiday, say researchers from Georgetown University Medical Center. They say the changes indicate brain functioning is more streamlined after an exercise intervention because less of the brain's resources is devoted to processing bothersome fibromyalgia perceptions such as pain.
The study, presented at the Society of Neuroscience's annual meeting, Neuroscience 2011, used functional MRI scans to assess changes in the brain. Researchers observed a decrease in brain activity in areas responsible for memory and pain control after fibromyalgia patients took part in an exercise regimen.
"The decreased brain activity we see in the area of cognition suggests that the brain is working more efficiently," explains Brian Walitt, M.D. M.P.H., director of the Fibromyalgia Evaluation and Research Center at Georgetown University Medical Center and senior study author. "We also see less brain activity in areas responsible for pain processing which might be aiding that efficiency." Walitt cautions that more research needs to be conducted before suggesting a change in clinical care for fibromyalgia.
Fibromyalgia is a medical disorder characterized by widespread pain, fatigue, disordered sleep, and cognitive changes. It is regarded as an interoceptive disorder in that it has no apparent cause, Walitt says. "In conditions like this, the body perceives something by mistake." The pain is not psychosomatic, but is real and likely produced by the central nervous system, he says.
To that end, the research team used fMRI to "provide a definitive measure of cognitive functioning, so that we can more scientifically measure the effect of exercise," says Manish Khatiwada, M.S., who will be presenting the results. "This is a novel approach to the study of fibromyalgia." (Khatiwada is working in the laboratory of co-author John VanMeter, Ph.D., director of the Center for Functional and Molecular Imaging.)
For this study, the researchers enrolled eighteen women with fibromyalgia, and gave them a baseline fMRI to assess working memory and questionnaires about their well-being and pain while they were on medication. They then were told not to use their medications for a "washout" period, and had a second fMRI and memory testing. After six weeks, they had another assessment. The final scan was taken after the volunteers engaged in a six-week period of exercise, which involved three 30-minute sessions of aerobic exercise each week with a trainer.
Memory and pain typically worsen in patients after stopping their medication — which was the experience of patients in this study. After six weeks of exercise, however, patients reported an improvement in overall well-being. However, their performance in the memory task did not change significantly when compared to their baseline study measurements. Despite a change in memory test performance, brain activity in the memory task and pain processing areas of the brain decreased.
"What we see is a less interference by pain activity which could be contributing to the decrease in activity in the memory section. Basically, the brain is using less energy for the same task," Walitt says.
More information: Presentation Title: Effect of aerobic exercise on working memory in fibromyalgia Location: Hall A-C
Abstract:
Introduction: Fibromyalgia (FM) is a disorder characterized by wide spread musculoskeletal pain and diffuse tenderness at multiple tender points that disproportionably affects women (Bartels 2009, Wolfe 1990). Previous studies have shown impairments in working memory, and long-term verbal memory in FM (Dick 2002, Park DC 2001). Aerobic exercise has been shown to improve the cognitive function, tenderness and disability of FM (Goldenberg 2008, Nichols 1994). The goal of this investigation was to determine the effect of aerobic exercise on working memory in FM using functional magnetic resonance Imaging (fMRI).
Methods: Nine female FM subjects (8 right handed, 1 left handed; age 45.8±10.60 years) who met the 1990 American College of Rheumatology criteria for FM were included in this study. The study consisted of 4 visits: 1) Baseline: on current FM medications, 2) Washout: off all FM medications for 3 half-lives, 3) No Treatment: 6 weeks after stopping FM medications, and 4) Exercise: after a 6 weeklong aerobic exercise intervention. At each visit an N-Back fMRI task (serial letter recognition with 0 and 2 back) was collected. Data was acquired on a Siemens 3T Tim Trio: TR/TE=2500/30ms, effective resolution 3.2mm3, and 47 slices. SPM5 was used to realign, spatially normalize, and smooth the data. A full factorial random-effects model was used to analyze changes in neuronal activity across visits using a model related to changes in their patient global impression change (PGIC) with an initial drop followed by steady improvement.
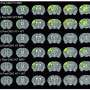
Results: The second-level model related to PGIC change across visits of the 2back > 0back contrast revealed increased activation in task-related areas: L Superior Medial Frontal, L Dorsal Lateral Prefrontal, R Mid Frontal, R Supplementary Motor, L Thalamus, L Caudate, L Inferior Parietal, Bi Superior Parietal (Fig 1 p<0.05 uncorrected).
Conclusions: Our results indicate that as the patients discontinue their current medication treatment and transition into the exercise treatment their subjective rating of change in pain initially increases and then decreases. Neuronal activity in areas recruited for an Nback working memory task follow an inverse pattern with an initial drop following medication cessation that increases on subsequent visits. These results are suggestive of the effect exercise on not only self report of global change in pain sensation in FM but also improvement in the network of cortical areas recruited in working memory. Thus, exercise may have benefit in both reducing FM symptoms and improving cognitive capacity.