Pill some day may prevent serious foodborne illness, scientist says
Modified probiotics, the beneficial bacteria touted for their role in digestive health, could one day decrease the risk of Listeria infection in people with susceptible immune systems, according to Purdue University research.
Arun Bhunia, a professor of food science; Mary Anne Amalaradjou, a Purdue postdoctoral researcher; and Ok Kyung Koo, a former Purdue doctoral student, found that the same Listeria protein that allows the bacteria to pass through intestinal cells and into bloodstreams can help block those same paths when added to a probiotic.
"Based on the research, it looks very promising that we would get a significant reduction in Listeria infections," said Bhunia, whose findings were published this month in the journal PLoS One.
Bhunia's earlier work showed that Listeria triggers intestinal cells to express heat shock protein 60 on their surfaces. That allows Listeria to bind to the intestinal cells using an adhesion protein and pass into them, acting as a sort of gateway to the bloodstream.
Once in the bloodstream, even small doses of Listeria can cause fever, muscle aches, nausea and diarrhea, as well as headaches, stiff neck, confusion, loss of balance and convulsions if it spreads to the nervous system. It can also cause abortion and stillbirth in pregnant women.
According to the U.S. Centers for Disease Control and Prevention, it sickens about 1,500 and kills 255 people each year in the United States and primarily affects pregnant women, newborns, older adults and those with weakened immune systems.
"We're seeing fewer Listeria infections, but the severity of those infections is still high," Amalaradjou said.
The researchers found that probiotics alone were ineffective in combatting Listeria, so they stole a trick from the bacteria's own playbook. By adding the Listeria adhesion protein to the probiotic Lactobacillus paracasei, they were able to decrease the number of Listeria cells that passed through intestinal cells by 46 percent, a significant decrease in the amount of the bacteria that could infect a susceptible person.
With the adhesion protein, Lactobacillus paracasei interacts with heat shock protein on the surface of intestinal cells just as Listeria would. The probiotic then attached to the intestinal cells, crowding out Listeria.
"It's creating a competition," Bhunia said. "If Listeria comes in, it doesn't find a place to attach or invade."
Bhunia said he could one day foresee the development of a pill or probiotic drink that could be given to at-risk patients to minimize the risk of Listeria infection.
The results came from tests on human intestinal cells. The next step would be animal testing. Bhunia said that would allow him to see whether different doses would have a greater effect.
More information: Recombinant Probiotic Expressing Listeria Adhesion Protein Attenuates Listeria monocytogenes Virulence In Vitro, PLoS One.
ABSTRACT
Background: Listeria monocytogenes, an intracellular foodborne pathogen, infects immunocompromised hosts. The primary route of transmission is through contaminated food. In the gastrointestinal tract, it traverses the epithelial barrier through intracellular or paracellular routes. Strategies to prevent L. monocytogenes entry can potentially minimize infection in high-risk populations. Listeria adhesion protein (LAP) aids L. monocytogenes in crossing epithelial barriers via the paracellular route. The use of recombinant probiotic bacteria expressing LAP would aid targeted clearance of Listeria from the gut and protect high-risk populations from infection.
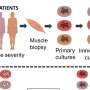
Methodology/Principal Findings: The objective was to investigate the ability of probiotic bacteria or LAP-expressing recombinant probiotic Lactobacillus paracasei (LbpLAP) to prevent L. monocytogenes adhesion, invasion, and transwell-based transepithelial translocation in a Caco-2 cell culture model. Several wild type probiotic bacteria showed strong adhesion to Caco-2 cells but none effectively prevented L. monocytogenes infection. Pre-exposure to LbpLAP for 1, 4, 15, or 24 h significantly (P<0.05) reduced adhesion, invasion, and transepithelial translocation of L. monocytogenes in Caco-2 cells, whereas pre-exposure to parental Lb. paracasei had no significant effect. Similarly, LbpLAP pre-exposure reduced L. monocytogenes translocation by as much as 46% after 24 h. LbpLAP also prevented L. monocytogenes-mediated cell damage and compromise of tight junction integrity. Furthermore, LbpLAP cells reduced L. monocytogenes-mediated cell cytotoxicity by 99.8% after 1 h and 79% after 24 h.
Conclusions/Significance: Wild type probiotic bacteria were unable to prevent L. monocytogenes infection in vitro. In contrast, LbpLAP blocked adhesion, invasion, and translocation of L. monocytogenes by interacting with host cell receptor Hsp60, thereby protecting cells from infection. These data show promise for the use of recombinant probiotics in preventing L. monocytogenes infection in high-risk populations.