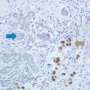
Heat-shock factor reveals its unique role in supporting highly malignant cancers
Whitehead Institute researchers have found that increased expression of a specific set of genes is strongly associated with metastasis and death in patients with breast, colon, and lung cancers. Not only could this finding help scientists identify a gene profile predictive of patient outcomes and response to treatment, it could also guide the development of therapeutics to target multiple cancer types.
The genes identified are activated by a transcription factor called heat-shock factor 1 (HSF1) as part of a transcriptional program distinct from HSF1's well-known role in mediating the response of normal cells to elevated temperature.
In normal cells, a variety of stressors, including heat, hypoxia, and toxins, activate HSF1 leading to increased expression of so-called heat-shock or chaperone proteins that work to maintain protein homeostasis in stressed cells. Scientists have known for some time that many cancer cells have higher levels of chaperones and that elevation of these proteins is important for survival and proliferation of tumor cells.
Now, however, researchers in the lab of Whitehead Member Susan Lindquist report that HSF1 supports cancers not only by increasing chaperones, but by unexpectedly regulating a broad range of cellular functions that are important for the malignant behavior of tumor cells. This activity allows for the development of the most aggressive forms of three of the most prevalent cancers—breast, lung, and colon. The findings, published this week in the journal Cell, build on earlier research from the Lindquist lab showing that elevated levels of HSF1 are associated with poorer prognosis in some forms of breast cancer.
"This work shows that HSF1 is fundamentally important across a broad range of human cancers, cancers of various types from all over the body turn on this response," says Sandro Santagata, a postdoctoral researcher in the Lindquist lab. "That's very interesting. It suggests how important HSF1 must be for helping tumors become their very worst."
In addition to confirming that this gene activation program differs from that associated with heat shock, the researchers found that in many tumors, it becomes active in virtually all of the tumor's cells.
"This demonstrates it isn't simply regions of microenvironmental stress within a tumor that drive HSF1 activity, but rather that HSF1 activation is wired into the core circuitry of cancer cells, orchestrating a distinct gene regulatory program that enables particularly aggressive phenotypes," says Marc Mendillo, a postdoctoral researcher in the Lindquist lab. "This suggests HSF1 itself could be a great therapeutic target."
Luke Whitesell, an oncologist and senior research scientist in the Lindquist lab, concurs that HSF1 is a conceptually appealing target for therapeutic intervention, noting that suppressing HSF1 for short periods of time should have minimal consequences on normal cells. However, he adds, actually developing such a drug could be problematic.
"Coming up with a drug that disrupts HSF1's interaction with DNA, which is how it activates all of these genes, that is going to be really tough," says Whitesell. "No one has come up with a clinically useful drug that directly interrupts a transcription factor's interaction with DNA yet. But there are ways to disrupt a transcription factor's function indirectly, as opposed to directly targeting the protein itself. What we have now from this research is a new view of the landscape and the possibilities for drug discovery and development that are out there."
More information: "HSF1 drives a transcriptional program distinct from heat shock to support highly malignant human cancers" Cell, August 3, 2012.