Two-faced drugs fight hidden killers
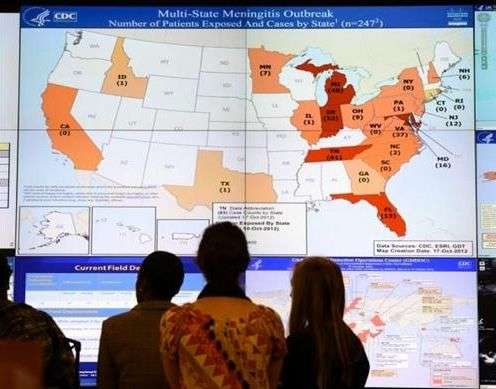
(Medical Xpress)—An outbreak of fungal meningitis recently resulted in one of the worst public health disasters in recent U.S. history. Thirty-two people died and more than 400 became ill after the New England Compounding Center distributed contaminated vials of injectable steroids.
Public health officials are clamoring for stricter regulation of so-called compounding pharmacies, which until now have flown under the radar of the Food and Drug Administration. Of major health concern in cases like this is the nature of the infections themselves. Hiding behind the blood-brain barrier, or BBB, a concept every first-year biology or psychology student is familiar with, these infections escape direct contact with most medications and require patients to endure long and sometimes unsuccessful treatment with antibiotics.
Steven Regen, University Distinguished Professor of chemistry, is working at the forefront of efforts to treat fungal meningitis that hides behind that barrier. Regen conducts research in the field of membranes and drug delivery with Vaclav Janout, senior research scientist, and Celine Bienvenu, postdoctoral research associate, both in the department of chemistry. With funding from the National Institutes of Health, they are seeking to develop a new class of drugs that can pierce the BBB and provide effective treatment for fungal meningitis and a host of other diseases in the brain.
A new paradigm for drug transport
"In a broader context," said Regen, "if we have any luck with our approach it could establish a new paradigm for the transport of many other drugs into the central nervous system."
The BBB consists of tightly packed endothelial cells that separate circulating blood from cerebrospinal fluid in the central nervous system. One of the greatest challenges facing medicinal chemistry is the search for drugs that can be transported across that barrier. Many classes of drugs with the potential for treating brain diseases (fungal and bacterial infections, malignant tumors, neurodegenerative diseases, etc.) have minimal effectiveness because of their limited ability to cross the BBB.
One example is amphotericin B (AmB), an antibiotic currently used to treat fungal meningitis. Because AmB does not readily cross the BBB, and because it is highly toxic, its overall effectiveness is limited.
Regen's team has been asked by NIH to create a new class of AmB agents based on what Regen calls molecular umbrellas. These structures are a novel class of amphiphiles, or chemical compounds whose exteriors are both hydrophobic and hydrophilic and thus ideal for crossing hydrophobic membranes like the BBB.
Dual conformational properties
What makes molecular umbrellas valuable, says Regen, is that they may be able to carry biologically active agents across the BBB in ways that have not previously been possible.
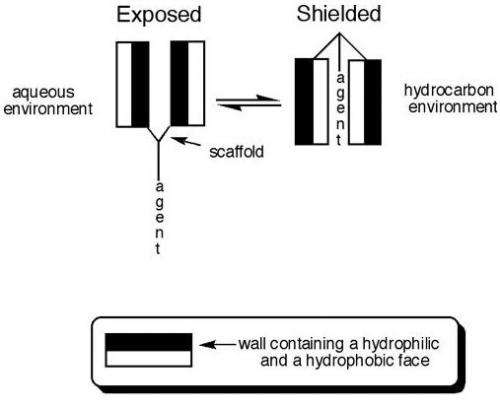
The innovative aspects of this research lie entirely with the unique conformational and transport properties associated with molecular umbrellas. In essence, molecular umbrellas are molecules composed of two or more walls attached to a central scaffold. When immersed in an aqueous environment, a molecular umbrella favors a conformation in which the hydrophobic faces point towards one another, to shield themselves from water.
Conversely, when immersed in a lipophilic environment, the molecular umbrella favors a conformation in which the hydrophilic faces point toward each other and the lipophilic faces point outward. In this case, the hydrophilic faces now become shielded from the external environment. Regen's team calls such behavior "molecular amphomorphism."
Regen's team will test the potential of molecular umbrellas that are chemically attached to AmB to kill fungal cells in cell culture and in animal models. These animal studies will be carried out by Professor John Perfect, a collaborator at Duke University School of Medicine, who is an expert in fungal infections. If, as expected, one or more of the molecular umbrella-AmB combinations prove more effective than simple AmB, there could be good reasons to explore other molecular umbrella-drug combinations for a variety of diseases, possibly even brain tumors.
At a more fundamental level, the research challenges the current dogma that drug transport is limited by molecular size and lipophilicity. In published work, Regen and his team have shown that very large and hydrophilic molecular umbrellas can enter live cells in cell culture experiments. They have also shown that they can cross model membranes that mimic cell membranes.
As they test new compounds, the researchers will learn whether the antibiotic supply in the brain speeds or slows depending on the size and structure of their molecular umbrellas.