Parkinson's patients advised to seek Deep Brain Stimulation treatment in early stages
People with Parkinson's disease who receive Deep Brain Stimulation (DBS) therapy in the early stages of the condition will benefit from a significant increase in quality of life, a revolutionary study from The New England Journal of Medicine has found.
World-leading neurologist and lead clinician Professor Peter Silburn from the Asia-Pacific Centre for Neuromodulation (APCN), a joint initiative of The University of Queensland (UQ) and St Andrew's Hospital, said the results published today in the medical journal would transform the way we treat people with Parkinson's disease.
"Before the release of this study, a typical patient with Parkinson's disease would need to wait around 10 years or until their motor complications could no longer be treated successfully with medicine alone, before DBS surgery was considered an option," Professor Silburn said.
"This study has confirmed the best medical practice for a person with Parkinson's disease is to perform DBS surgery around 4 to 7 years into the condition, as opposed to waiting until the medications stop working."
Participants in the EARLYSTIM trial had been experiencing symptoms of Parkinson's disease for an average of 7.5 years – about five years less than participants in earlier trials – allowing researchers to test the benefits of DBS therapy when motor fluctuations and dyskinesia are of recent onset and occupational and psychosocial competence is still maintained.
Key findings from these participants two years after receiving DBS therapy include:
- 26 percent improvement in their disease-related quality of life
- 53 percent improvement in motor skills
- 30 percent improvement in activities of daily life (speech, handwriting, dressing and walking)
- 61 percent improvement in levodopa-induced complications (including dyskinesias and motor fluctuations)
- 39 percent reduction in daily levodopa equivalent dosage.
Participants who did not undergo DBS surgery and received the best medical therapy only, experienced no improvement in their quality of life, no change in their motor skills, a 12 percent decline in their ability to perform daily activities, a 13 percent worsening in their levodopa-induced complications and a 21 percent increase in their daily levodopa equivalent dosage at two years.
As one of the world's top five centre's conducting DBS surgery, Professor Silburn said the APCN's responsibility to educate and train people in the delivery of DBS surgery has never been more important and patients should be aware of seeking advice from experienced DBS practitioners only.
"One thing that may hinder this study from being adopted earlier in Australia is that very few neurologists and neurosurgeons have been trained in performing DBS surgery," Professor Silburn said.
"Equally challenging, the results from this study need to filter their way through to referring doctors, including general practitioners and neurologists, so that DBS and referral to a DBS specialist are considered earlier in the course of the disease.
"The APCN has the privilege and responsibility to use education, research, clinical collaborations and outcomes to drive the findings of this study into the field, while advancing our understanding of the human brain and treatment therapies for patients with Parkinson's disease."
Professor Silburn hopes this study will serve as a paradigm shift in the way patients with Parkinson's disease think about their treatment options, dispelling the assumptions about being too old, too young, or too far along in the disease to be suitable for DBS surgery.
"My message to people diagnosed with Parkinson's disease is this- it doesn't matter what age you are, or how far along you are in the disease, you don't have to persist with the drugs, or wait until you're so bad that nothing else helps, before considering DBS surgery," Professor Silburn said.
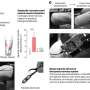
The video above is an animation showing how Medtronic Deep Brain Stimulation therapy works to help people living with Parkinson's disease, and other indicated movement disorders.
More information: www.nejm.org/doi/full/10.1056/ … ?query=featured_home