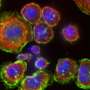
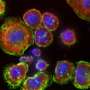
Fighting cancer with microgravity research
(Phys.org) —For lab-coated cancer biologists, peering through microscopes at stained tissue samples under fluorescent lights, the International Space Station may be the last thing that comes to mind. But 40 years of microgravity research proves cancer biologists may indeed want to look 220 miles up. Space provides physical conditions that are not possible on Earth, and as it turns out, those conditions may be ripe for studying cancer—along with a wide range of other diseases.
Cells
in the human body normally grow within support structures made up of proteins and carbohydrates, which is how organs—and tumors—maintain their three-dimensional shapes. In lab settings, however, cells grow flat, spreading out in sheets. Because they don't duplicate the shapes they normally would make in the body, they don't behave the way they would in the body, either. This poses problems for scientists who study cancer by examining
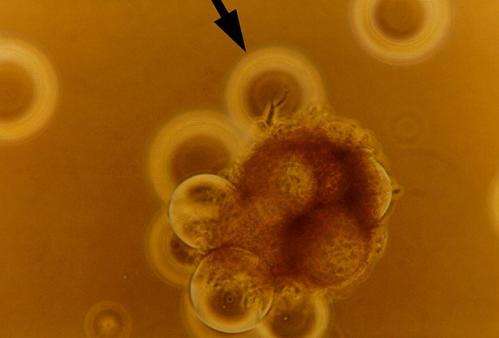
Scientists have devised several laboratory methods to mimic normal cellular behavior, but none of them work exactly the way the body does. In space, however, cells that are not inside a living organism, called in vitro cells, still arrange themselves into three-dimensional groupings, or aggregates. These aggregates more closely resemble what happens in the body. Cells in microgravity also can clump together more easily, and they experience reduced fluid shear stress—a type of turbulence that can affect their behavior. All these factors can help scientists study cell behavior—and how changes in that behavior can lead to cancer—in a state more closely resembling cells in the body.
"So many things change in 3-D, it's mind-blowing—when you look at the function of the cell, how they present their proteins, how they activate genes, how they interact with other cells," said Jeanne Becker, Ph.D., a cell biologist at Nano3D Biosciences in Houston and principal investigator for the CBOSS-1-Ovarian study. "The variable that you are most looking at here is gravity, and you can't really take away gravity on Earth. You have to go where gravity is reduced."
Becker is the author of a recent paper in Nature Reviews Cancer that surveys the past four decades of cell biology research in microgravity, and how the findings continue to inform cancer research on Earth. Starting with Skylab in the 1970s and leading up to current in-orbit investigations, Becker and co-author Glauco R. Souza highlight nearly 200 scientific papers drawn from space-based experiments and investigations.
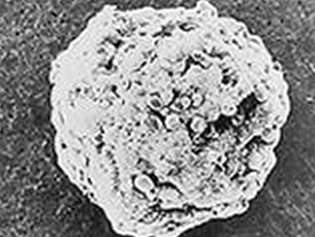
Experiments on the space shuttle, Russian vehicles and the space station have shown changes in immune cells, including changes in cell-signaling cytokines, indicating the immune system is suppressed in microgravity. Even the architecture of cells changes in microgravity, with changes to cell walls, internal organization and even their basic shapes. In space, according to Becker's review, cells are more round.
Other studies have shown many changes in genetic expression. During an investigation on the STS-90 mission aboard space shuttle Columbia in 1998, cells were cultured for six days and returned to Earth for analysis. Afterward, an examination of 10,000 genes revealed the expressions of 1,632 genes were altered in microgravity, relative to ground controls. This was the first experiment to show reduced gravity can affect a wide range of genes.
Aboard Columbia during its STS-107 mission, prostate cancer and bone cells grew in a three-dimensional structure inside the Bioreactor Demonstration System (BDS–05). Early indications showed large aggregates of cells, indicating large growth, Becker said. But the study was lost, along with the shuttle and its crew, during re-entry on Feb. 1, 2003.
The Cellular Biotechnology Operations Support System (CBOSS-01-Ovarian) investigation aboard the space station contains a cell incubator that can grow 3-D clusters of cells, and scientists have used it to examine changes to human colon, ovarian and other cancer cells. In one recent result, Becker noted reduced production of cytokines in a human Muellerian ovarian (LN1) tumor cell line. Cytokines are small proteins that are secreted to mediate and regulate immunity and inflammation. Understanding changes in production of these proteins, and the changes in cell signaling that contribute to those production changes, could help researchers understand the mechanisms of tumor cell development.

Although cells grow in three-dimensional structures in microgravity, they don't possess blood vessels that can provide oxygen and nutrients, so the cells at the center of an aggregate will likely die. But that's still not a disadvantage, Becker said. Bulky tumors also have areas of dead tissue near their centers, which coincides with a slow cancer growth rate."You also have nearby cells that are not dead, but they're not really cycling. They are very much still cancer, and they can develop increased areas of chemo resistance," said Becker. "That mirrors exactly what you see in human cancer."
Even while they're sitting at the lab bench, researchers could reach new heights using the station's microgravity environment, Becker said. "I've had the chance to see firsthand the things that can happen. It's pretty amazing. It's a shame to not take full advantage of this platform for discovery," she said. "It's the only lab of its kind; that's it. And now is the time, because the station is entirely finished and available."
In recent years, research on Earth has caught up with 3-D cell structures. Investigations examining cancer cells and other tissues use a collagen gel matrix, which suspends cells in 3-D. Combining these techniques with the resources available in microgravity may inform entirely new approaches for studying cancer. Ultimately, microgravity- and Earth-based research could help scientists pinpoint the cellular changes that lead to cancer and possibly find new ways to prevent them, leading to new treatments that could enhance the quality of life for patients with the disease.
More information: www.nature.com/nrc/journal/v13 … n5/full/nrc3507.html