Neurological testing limited in diagnosing disc herniation
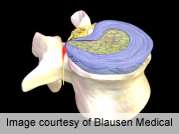
(HealthDay)—Neurological testing procedures have limited diagnostic accuracy for detecting disc herniation with suspected radiculopathy, according to a review and meta-analysis published in the June issue of The Spine Journal.
Nezar H. Al Nezari, P.T., M.Phty., from the University of Otago in New Zealand, and colleagues conducted a literature review to examine the diagnostic accuracy of neurological examination to detect lumbar disc herniation with suspected radiculopathy. Fourteen studies that investigated three standard neurological examination components (sensory, motor, and reflexes) were included.
The researchers found that, using pooled data from sensory testing, there was low diagnostic sensitivity for surgically and radiologically confirmed disc herniation (0.40 and 0.32, respectively) and for identification of a specific level of disc herniation (0.35), while specificity was moderate for all three reference standards (0.59, 0.72, and 0.64, respectively). Pooled diagnostic sensitivities were similarly low with motor testing for paresis (0.22 for surgically and 0.40 for radiologically determined disc herniation), while specificity was moderate (0.79 and 0.62, respectively). For surgically determined disc herniation, motor testing for muscle atrophy resulted in a pooled sensitivity of 0.31 and specificity of 0.76. For surgically and radiologically confirmed levels of disc herniation, the pooled sensitivities for reflex testing were 0.29 and 0.25, respectively, while the specificities were 0.78 and 0.75, respectively. For all neurological examination components the pooled positive likelihood ratios ranged from 1.02 to 1.26.
"This systematic review and meta-analysis demonstrate that neurological testing procedures have limited overall diagnostic accuracy in detecting disc herniation with suspected radiculopathy," the authors write.
More information:
Abstract
Full Text (subscription or payment may be required)
Health News
Copyright © 2013