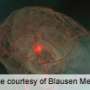
Decision-making tool may help rule out brain hemorrhage for patients in emergency department
Researchers have developed a simple clinical decision rule that may help doctors identify patients with headache in the emergency department who have subarachnoid hemorrhage (bleeding in a certain area of the brain), according to a study in the September 25 issue of JAMA.
"Headache accounts for approximately 2 percent of all emergency department visits, and subarachnoid hemorrhage is one of the most serious diagnoses, accounting for only 1 percent to 3 percent of these headaches. Although the decision to evaluate patients with new neurologic deficits is relatively straightforward, it is much more difficult to determine which alert, neurologically intact patients who present with headache alone require investigations—yet such patients account for half of all subarachnoid hemorrhages at initial presentation," according to background information in the article.
A clinical decision rule is a tool that uses 3 or more variables from the history, examination, or simple tests to predict a diagnosis for a patient. These rules help clinicians make diagnostic or treatment decisions. The investigators had previously developed three clinical decision rules for use in patients with headache to determine which patients require investigation (imaging, lumbar puncture) for subarachnoid hemorrhage.
Jeffrey J. Perry, M.D., M.Sc., of the Ottawa Hospital Research Institute, Ottawa, Canada, and colleagues further studied the 3 rules in a group of neurologically intact patients with acute headache at 10 Canadian emergency departments from April 2006 to July 2010 to determine which might be most useful and accurate.
Among 2,131 adult patients with a headache peaking within 1 hour and no neurologic deficits, 132 (6.2 percent) had subarachnoid hemorrhage. The researchers found that information about age, neck pain or stiffness, witnessed loss of consciousness, onset during exertion, "thunderclap headache" (defined as instantly peaking pain) and limited neck flexion on examination (defined as inability to touch chin to chest or raise the head 3 inches off the bed if supine [lying face upward]), was 100 percent sensitive (detected all cases), but only 15.3 percent specific (designated many patients without SAH as possibly having it). The authors named the rule the Ottawa SAH (subarachnoid hemorrhage) Rule.
The authors write that the rule may provide evidence for physicians to use in deciding which patients require imaging to decrease the relatively high rate of missed subarachnoid hemorrhages.
"These findings only apply to patients with these specific clinical characteristics and require additional evaluation in implementation studies before the rule is applied in routine emergency clinical care."
David E. Newman-Toker, M.D., Ph.D., of the Johns Hopkins University School of Medicine, Baltimore, and Jonathan A. Edlow, M.D., of Harvard Medical School, Boston, write in an accompanying editorial that "future studies should seek to validate the Ottawa SAH Rule using larger samples."
"Realistically, though, this may require use of administrative data and imputation of missing results. The rule should also be studied for the effect on patient outcomes as part of a clinical care pathway for headache diagnosis, ideally with direct comparison to an alternate care pathway based on the computed tomography-lumbar puncture rule. While awaiting further scientific advances, clinicians may find the refined Ottawa SAH Rule helpful to guide diagnostic decisions, but they should limit its use to patients with acute headache who are similar to those among whom the rule has been evaluated."
More information: doi:10.l001/jama.2013.278018 , doi:10.l001/jama.2013.278019