'Diabetic flies' can speed up disease-fighting research
In a finding that has the potential to significantly speed up diabetes research, scientists at the University of Maryland have discovered that fruit flies respond to insulin at the cellular level much like humans do, making these common, easily bred insects good subjects for laboratory experiments in new treatments for diabetes.
The common fruit fly Drosophila melanogaster looks like a sesame seed with wings, produces offspring by the thousands, and lives for around a month. These creatures don't resemble humans in any obvious way, but they share more than sixty percent of our genetic code. And scientists like UMD's Leslie Pick and Georgeta Crivat are finding that those similarities control basic biological processes that work alike in both species.
Drosophila melanogaster is easy to breed, raise and study in the laboratory, so it's widely used in research. Pick, chairman of the UMD Entomology Department, conducts experiments that use information about the fruit fly's relatively simple genome to illuminate biological processes in humans. Her recent research focuses on whether fruit flies use the hormone insulin the same way humans and other mammals do.
"We hope to use all the genetic tools we have available for flies, and the fact that we can breed them in huge numbers, very fast, to set up efficient screening tests for assessing new diabetes treatments," Pick said.
In a new study published Nov. 6 in the peer-reviewed online journal PLOS One, Pick and her co-authors found the basic mechanisms that humans use to regulate blood sugar – the process that goes awry in diabetes – are indeed shared with flies.

In humans, insulin controls the production and movement of glucose, the form of sugar that fuels mammalian cells. The movement of glucose into individual cells begins when insulin binds to a specialized insulin receptor on a cell. That causes a sugar transporter called GLUT4 to move from the cell interior to its membrane, allowing glucose to flow through the membrane, moving from the bloodstream into the cell. In diabetics, this process fails and sugar accumulates in the blood. In the main types of diabetes - Type 1, in which the body cannot produce insulin, and Type 2, in which the cells stop responding to insulin – high blood sugar levels can gravely damage many organs. The disease is one of the world's most serious health problems.
Fruit flies' systems are very different than humans. Glucose is not their main form of sugar, and they don't have blood like mammals do, so researchers were not sure whether insulin played a role in their cells that is similar to humans. But in a 2009 experiment, Pick and colleagues used genetic engineering techniques to disable five insulin-like fruit fly genes.
The resulting "diabetic flies" had many symptoms of diabetes in humans, Pick said. "They were very, very small and sluggish; they had decreased body fat and higher levels of circulating blood sugar; and they did not reproduce very well." Other researchers trying to understand diabetes have performed similar experiments on mammals, which usually did not survive the genetic alteration, Pick said.
"The flies are not fine, but they do live," Pick said. That meant more diabetes-related experiments, using flies instead of mammals, might be possible.
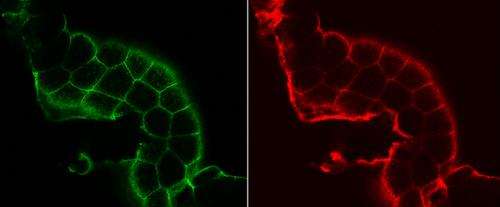
To be sure, the researchers needed to know whether the cellular processes taking place were the same in both species. Pick and her colleagues turned to Samuel Cushman of the National Institutes of Health, the co-discoverer of the glucose transport process involving GLUT4 in humans. Combining their expertise, the two research teams inserted GLUT4 into fruit flies, using a fluorescent tag to mark the GLUT4 molecules.
To the scientists' surprise, although this protein is foreign to the fruit flies, their cells moved GLUT4 to the cell membrane exactly as human cells do in response to insulin. Under a high powered microscope that picks up the fluorescent GLUT4,"You can actually track its movement onto the cell membrane."
"It's pretty amazing," Pick said. "We hoped that would happen, but there are so many differences between flies and mammals that we ourselves were skeptical."
The researchers' next step is to find the sugar transporter that fills the role of GLUT4 in fruit flies, Pick said, and "to use the fly model to see if we can screen for compounds that promote sugar uptake, alone or working together with insulin, to treat diabetes more effectively."
More information: Georgette Crivat, Vladimir A. Lizunov, Caroline R. Li, Karin Stenkula, Joshua Zimmerberg, Samuel W. Cushman and Leslie Pick, "Insulin stimulates translocation of human GLIUT4 to the membrane in fat bodies of transgenic Drosophila melanogaster," published in PLOS One Nov. 6, 2013. dx.plos.org/10.1371/journal.pone.0077953

















