Can the body have too much iron?

Many people are aware that low levels of iron in their body can lead anaemia, with symptoms such as fatigue. But few realise that too much iron can result in a potentially fatal condition.
Normally, if we have enough iron in our body, then no further iron is absorbed from the diet, and our iron levels remain relatively constant.
But the body also has no way of excreting excess iron. In a condition called hereditary haemochromatosis, the most common cause of iron overload, the mechanism to detect sufficient iron in the body is impaired and people can go on absorbing iron beyond the normal required amount.
Untreated, haemochromatosis can result in scarring to the liver (cirrhosis), liver cancer, damage to the heart and diabetes. These problems are the result of excess iron being deposited in the liver, heart and pancreas. Haemochromatosis can also cause non-specific symptoms such as fatigue, loss of libido and arthritis. In some, it results in a shortened lifespan.
The most common cause of hereditary haemochromatosis is a mutation received from both parents, in a gene called HFE.
Around one in every 200 Australians of European heritage have a double dose of this gene fault and are at risk of developing the disorder. Haemochromatosis is much less common among people who aren't of European ancestry.
Approximately 80% of men and 60% of women who have inherited this gene fault from both parents develop high iron levels. And of those who do, up to 40% of men and 10% of women will develop health problems.
Diagnosis
Actual blood iron levels are generally normal in those with haemochromatosis, as excess iron in the body is stored in tissues like the liver. So haemochromatosis is diagnosed by testing blood iron indices called transferrin saturation and serum ferritin levels.
Transferrin is a protein that transports iron around the body; ferritin is a protein that stores iron. The more iron in the body, the more ferritin that is made. Those with the haemochromatosis generally have high transferrin saturation and serum ferritin levels.
These proteins are very important in minimising tissue damage from iron, as iron that is not stored in ferritin or bound to transferrin is very toxic to cells.
If abnormal iron indices are identified, then genetic testing is usually the next step. Sometimes a liver biopsy is also required, to assess the degree of excess iron and whether there is permanent scarring of the liver.
There is debate among experts over whether everybody should undergo genetic testing for the disorder, even if they don't display symptoms.
Those who argue for blanket screening claim that if a person is at risk, knowledge of their condition will allow them to have their ferritin levels monitored, and they can seek treatment to prevent severe problems.
Arguments against the practice include the high cost of genetic screening, and the fact that many people who have the genetic risk don't go on to develop the disorder.
Treatment
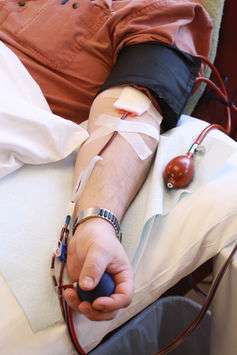
Donating blood is the primary form of treatment for haemochromitosis. Red blood cells contain haemoglobin, which is very high in iron – removing red blood cells therefore removes iron.
Once iron levels are normalised, a person generally needs to make two to four blood donations per year to maintain normal iron levels. Blood donated by people with haemochromitosis can generally be used in transfusions with no problems.
While there's no doubt that people with very high iron levels due to haemochromatosis require treatment through donating blood, the evidence is less clear for those with only slightly elevated iron levels.
A research study call Mi-iron is underway in Melbourne, Brisbane and Perth to examine whether there are benefits to treatment when there is only moderate iron excess.
In this study, individuals will either have their iron levels normalised or left untreated without the person knowing which is the case (there's more information here about how this is achieved). Various symptoms are being assessed before and after the intervention to see if people with haemochromatosis who don't have severely elevated iron levels benefit from treatment.
Media campaigns may encourage us to eat more red meat, in part to make sure that we get enough iron. But with haemochromatosis, there can be too much of a good thing.
This story is published courtesy of The Conversation (under Creative Commons-Attribution/No derivatives).
![]()