Understanding pain: Can the brain provide all the answers?

We now know that there's much more to pain than simply what is happening in the painful body part, and attention has turned to the role of the brain. But not even this mysterious organ can tell us everything we need to know about pain, at least not yet.
You may wonder why the brain is part of the discussion about pain at all. After all, we're not talking about a brain disease such as Alzheimer's or stroke.
But we think that the brain is actually the best place to look when trying to understand pain; after all, pain is a purely subjective experience.
The problem is that pain cannot be "seen". While a flinch, a limp, or a grimace may provide us with clues, ultimately we only know that someone is in pain if they tell us they are.
And it doesn't necessarily make sense to only consider the part of the body that's sore – sometimes people report pain in a body part that no longer exists, known as phantom limb pain.
Just as not all pain arises as a result of an injury to a body part, not all injuries cause pain.
The brain interprets sensory information from the body according to the present context; incoming messages are evaluated concurrently with past experiences, memories, thoughts, and even how the painful body part is perceived. The same injury may cause us pain one day, and no pain the next.
Critically, pain is only experienced if the brain concludes, from this complex interplay, that there's potential for harm or danger to the body.
And many researchers around the world are investigating the function of the brain, or its activity, with different neuroimaging tools.
The most common of these tools is a functional magnetic resonance imaging (fMRI) scanner. New technologies like this provide us with exciting opportunities if we use them to answer important questions, using rigorous methods.
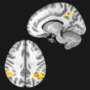
Recent advances in statistical methods have led a US research team to find the answer to a very important question – can we see pain in the brain?
These researchers have discovered a neurologic signature of physical pain that is highly sensitive. These patterns of brain activity predicted pain with over 90% accuracy (positive predictive value) in the group of people scanned.
But can a brain scan tell the whole pain story?
Despite this being perhaps the closest we've ever come to "seeing" pain, there are some things about the study we should keep in mind.
The research used a particular type of stimulation – placing hot thermodes on the skin of the forearm – to produce pain in healthy pain-free participants.
One can assume that the study participants knew they were involved in an experiment, that the pain they were experiencing was going to be short-term, and that the experiment could be stopped if needed.
A major issue then is just how generalisable these findings are. Would we see the same neural signature for pain if we were to scan the brain of someone with a 30-year history of low back pain? Would we capture the complex interplay that has led to the construction of pain in that person, at that time?
This leads to question of whether it is, in fact, worth embarking on a quest to find an objective measure for something that is so fundamentally subjective. It may not be valid or useful to search for a biomarker for pain as we would for cancer or heart disease.
And there's another, very significant, issue to consider.
Identifying a brain-based pain signature has been promoted as a step forward in understanding the pain experience of people who cannot communicate their pain. But we should take a very cautious approach to putting this into practice.
It's not uncommon, even though we know so much about the disconnect between tissue injury and pain, for chronic pain sufferers to be accused of feigning pain simply because no pathology can be seen on an X-ray.
We must avoid simply moving these errors of interpretation from scans of the back to scans of the brain, or people suffering pain will continue to be mistrusted.
To this end, the lead author of the US study rightly warned against the use of a neurologic signature for pain as a "lie detector".
The lack of an objective measure for pain is often seen as a barrier to understanding pain. But pain provides neuroscientists with a remarkable opportunity to investigate how the brain construes a complex experience.
By identifying a neural signature, the US study discussed above has made significant progress towards seeing pain in the brain. Research like this moves us forward on the fascinating road towards understanding pain and brain function.
But answers to questions about a complex and subjective experience are likely to come from more than the identification of a neural signature.
This story is published courtesy of The Conversation (under Creative Commons-Attribution/No derivatives).
![]()