NIH study describes new method for tracking T cells in HIV patients
A team of researchers has reported a novel method for tracking CD4+ T cells in people infected with HIV. CD4+ T cells are critical for immune defense against an array of pathogens and are a primary target of HIV. In the study, researchers used a unique, replication-incompetent (defective) form of HIV identified in a patient in the early 1990s.
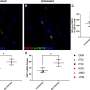
The defective virus had integrated into the genome of a single CD4+ T cell. Like a barcode, this "provirus" marked the originally infected CD4+ T cell and its progeny, enabling researchers to track its lineage for 17 years. This new method allows scientists to distinguish dividing cells from dying ones, something that has not been possible with existing labeling techniques, but is essential for studying how immune cells survive HIV infection.
The study, published in the online issue of AIDS, was conducted by Hiromi Imamichi, Ph.D., H. Clifford Lane, M.D., and others in the Laboratory of Immunoregulation at the National Institute of Allergy and Infectious Diseases (NIAID), part of the National Institutes of Health. The cell lineage is part of a subset of CD4+ T cells called "effector memory" (TEM) cells. This distinction is significant because it is currently believed that TEM cells last for only days or weeks. The NIAID investigators demonstrated that this subpopulation of T cells can persist for at least 17 years.
The researchers also observed in the blood cells of patients a higher frequency of defective HIV proviruses than what has been reported in previous work. Although these defective variants cannot produce an infectious virus, many retain the ability to generate small pieces of HIV, leading the researchers to speculate that these "foreign materials" within CD4+ T cells may play a key role in the ongoing immune activation that is characteristic of HIV infection, including in patients with "undetectable" virus in their blood.
More information: H. Imamichi et al. Lifespan of effector memory CD4+ T cells determined by replication-incompetent integrated HIV-1 provirus. AIDS. DOI: 10.1097/QAD.0000000000000223 (2014).