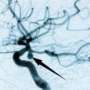
Brain surgery through an incision the size of a pinprick
The difference between having a brain aneurysm treated the old way and a new way was aptly described as "the nutcracker" vs. "the TripTik" by a patient of Andrew Ringer, MD, professor of neurosurgery at the University of Cincinnati College of Medicine.
The patient experienced both, and he clearly preferred the TripTik.
During the first procedure, Ringer opened the man's skull and placed a clip on the threatening aneurysm. In the second procedure, he made a tiny incision in the man's groin and threaded a catheter up to his brain, then filled the aneurysm with tiny coils.
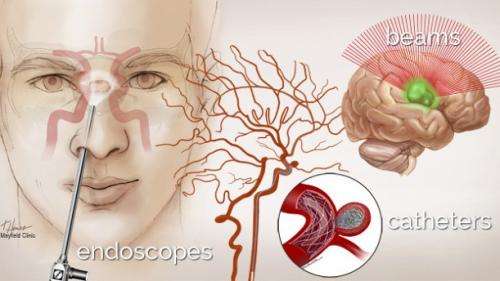
Reaching the brain through an incision the size of a pinprick is just one example of the direction neurosurgery is taking. A growing number of patients who undergo surgery at UC Health University of Cincinnati Medical Center (UCMC) for aneurysms, stroke, brain tumors, Parkinson's disease and epilepsy find that they qualify for a minimally invasive treatment that involves 1) endovascular surgery (the "TripTik" through the bloodstream); 2) small "keyhole" incisions in the skull, eyelid or nose; or 3) radiation therapy that involves no incision at all.
This means that, increasingly, neurosurgeons are less apt to open the skull—a procedure called a craniotomy—and are more apt to make repairs by threading catheters, beaming radiation or maneuvering long narrow tools called endoscopes.
"Not all patients qualify for minimally invasive techniques," says Ringer, a neurosurgeon at the Comprehensive Stroke Center at the UC Neuroscience Institute (UCNI) and the Mayfield Clinic. "The type and location of the surgical problem, along with the patient's overall health and age, are factors we must take into consideration. But the growing number of patients who qualify for minimally invasive procedures can reap genuine benefits."
Those benefits include:
- Smaller incisions
- Potential to avoid general anesthesia
- Less pain and blood loss
- Lowered risk of infection
- Faster recovery
- Reduction or elimination of scarring
- Shorter hospital or outpatient stay
In the area of cerebrovascular disease, which includes brain aneurysms, arteriovenous malformations and blocked arteries, neurosurgeons like Ringer are teaming up with interventional radiologists to use endovascular (within-the-artery) procedures to treat disorders of the arteries and veins of the brain by filling them with glue and coils or by neutralizing them with stents, balloons and flow-diverting devices.
"Through several impressive advancements in technology, we are now able to treat these disorders using precise mapping—like the GPS in your car—and advanced imaging that make exposure and repair so accurate that we can often avoid the large surgical incisions required in years past," Ringer says.
"In fact, many of these disorders can be treated from within the artery or vein itself. A tiny needle stick gives us access to the inside of an artery in the leg, which we then use as a highway to drive the catheter to the arteries in the brain so that we never have to open the patient's head at all."
Meanwhile, skull base surgeons have charted new paths to pituitary and meningioma tumors located at the base of the skull. Neurosurgeons and ear, nose and throat surgeons (otolaryngologists) combine to remove these tumors by approaching them through the nose or the roof of the mouth.
In one recent case at UCMC, Lee Zimmer, MD, PhD, associate professor of otolaryngology and a UC Health otolaryngologist, inserted a long, tube-like instrument with a light and tiny camera into one nostril and made an incision at the back of the nasal cavity. After Zimmer reached the tumor, a neurosurgeon removed it with another long, slender instrument that he inserted into the patient's other nostril. The entire procedure took 45 minutes.
Mario Zuccarello, MD, Professor and Frank H. Mayfield Chair for Neurological Surgery, refined a transorbital (eyelid) approach to selected aneurysms and tumors in the anterior (front) part of the brain. This approach, Zuccarello says, is "an effective, cosmetically beneficial, and minimally invasive option" in the treatment of hard-to-reach aneurysms and tumors of the skull base.
Some patients with Parkinson's disease or epilepsy can be effectively treated with deep brain stimulation procedures, which also require only the smallest of incisions.
"The opening in the bone is just a drill hole, about the size of a quarter," says George Mandybur, MD, associate professor of neurosurgery and a Mayfield Clinic neurosurgeon. "Most patients with Parkinson's disease who undergo deep brain stimulation surgery are in an awake state and experience minimal discomfort. Patients never need transfusions with this surgery."
An electrode is inserted through the tiny opening in the skull and into a movement-controlling area deep within the brain. The lead (wire) is then threaded under the skin and connected to a battery-powered pulse generator, similar to a heart pacemaker, which is implanted near the collarbone.
In the future, Mandybur says, this powerful tool will allow surgeons to treat other neurologic disorders, including Alzheimer's disease, eating disorders and psychiatric disorders.
A different type of minimally invasive brain stimulation, called vagus nerve stimulation, can help reduce the frequency of seizures in people with drug-resistant epilepsy. The procedure involves implanting a lead around the vagus nerve in the neck. The lead, connected to a pulse generator implanted under the skin, sends electrical signals that travel along the vagus nerve to the brain.
Least invasive are radiosurgery and radiotherapy, which require no incision at all. Both involve destroying a tumor or diseased tissue by bombarding it with targeted beams of radiation. Radiosurgery uses high doses of radiation in a single or small number of treatments, while radiotherapy uses lower doses of radiation given in as many as 30 to 35 treatments. Radiation works by damaging the DNA inside cells and making them unable to divide and reproduce, therefore causing them to die.
John Breneman, MD, professor emeritus of radiation oncology and associate director of the Brain Tumor Center at UCNI, likens the experience to getting an X-ray. "There is no discomfort and no bleeding," he says. "Treatments typically last less than an hour, and patients almost always go home the same day."