July 22, 2014 report
Study reveals nervous system's role in asthma attacks
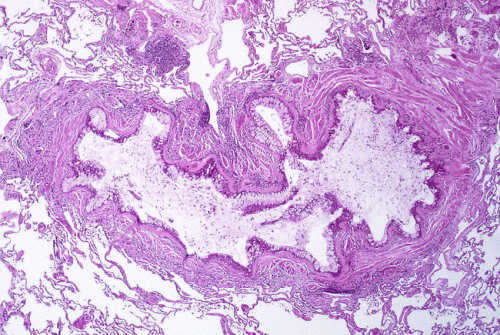
(Medical Xpress)—Asthma is a debilitating condition that kills 250,000 people around the world each year. People with asthma have hyperreactive airways and thickened lung walls obstructed with mucus. During an asthma attack, which could be fatal, airways constrict even further in the presence of a trigger, such as pollen, dust mites or a viral infection. Current asthma therapies treat asthma attacks as immune responses and focus on immune system suppression. However, a study by Dimitri Trankner of Howard Hughes Medical Institute in Virginia and his colleagues, published in the Proceedings of the National Academy of Sciences, shows that sensory neurons control bronchial hyperactivity.
Scientists know the immune system plays an important role in asthma. However, treatments that suppress the immune response and relieve inflammation do not control asthma symptoms completely. This indicates that asthma involves an additional mechanism.
Trankner and his team thought this mechanism might be nervous system activity. Sensory neurons in the vagal ganglia moderate respiratory responses such as coughing, and earlier studies have shown that the nervous system modulates asthma symptoms.
To test their hypothesis, the researchers genetically engineered mice with different groups of inactive neurons. They gave the mice an allergy to ovalbumin, egg white protein. This allergy causes asthma-like symptoms: airway hyperreactivity and constriction of the airways.
When exposed to ovalbumin, all but one group of mice experienced these symptoms. In the asymptomatic mice, nerve cells that express a receptor called transient receptor potential vallinoid 1 (TRPV1) were inactive. While these mice did not exhibit asthma-like symptoms, their immune systems did respond to the allergen; they produced ovalbumin-specific immunoglobulins and accumulated leukocytes in their lungs.
Deactivating TRPV1-expressing neurons in the vagal ganglia, but not in other parts of the body, still resulted in the suppression of asthma symptoms.
When the researchers stimulated TRPV1-expressing neurons in mice allergic to ovalbumin, bronchoconstriction worsened, even when no ovalbumin was present. This response did not occur in mice without the allergy, suggesting that an allergy primes the immune system to send neuron-sensitizing signals; sensitized neurons then cause asthma symptoms when stimulated.
Trankner's team thought a chemical known as sphingosine-1-phosphate (S1PR3), found in the lungs of ovalbumin-sensitized mice and implicated in the development of asthma, might be involved in signaling. When they injected the mice with an S1PR3 agonist, all of the mice, except those that did not express TRPV1, experienced airway hyperactivity, even without ovalbumin exposure. This suggests that lung inflammation leads to the release of chemicals that sensitize sensory neurons, which then cause asthma attacks. The researchers think new asthma therapies could target these neurons.
More information: Population of sensory neurons essential for asthmatic hyperreactivity of inflamed airways, Dimitri Tränkner, PNAS, DOI: 10.1073/pnas.1411032111
Abstract
Asthma is a common debilitating inflammatory lung disease affecting over 200 million people worldwide. Here, we investigated neurogenic components involved in asthmatic-like attacks using the ovalbumin-sensitized murine model of the disease, and identified a specific population of neurons that are required for airway hyperreactivity. We show that ablating or genetically silencing these neurons abolished the hyperreactive broncho-constrictions, even in the presence of a fully developed lung inflammatory immune response. These neurons are found in the vagal ganglia and are characterized by the expression of the transient receptor potential vanilloid 1 (TRPV1) ion channel. However, the TRPV1 channel itself is not required for the asthmatic-like hyperreactive airway response. We also demonstrate that optogenetic stimulation of this population of TRP-expressing cells with channelrhodopsin dramatically exacerbates airway hyperreactivity of inflamed airways. Notably, these cells express the sphingosine-1-phosphate receptor 3 (S1PR3), and stimulation with a S1PR3 agonist efficiently induced broncho-constrictions, even in the absence of ovalbumin sensitization and inflammation. Our results show that the airway hyperreactivity phenotype can be physiologically dissociated from the immune component, and provide a platform for devising therapeutic approaches to asthma that target these pathways separately.
© 2014 Medical Xpress