Study finds a new approach to tackle drug resistance in hematologic malignancies
Treating hematologic malignancies upfront with a combination of drugs based on the vulnerabilities of tumors as they evolve may be a viable strategy to avoid drug resistance, according to data presented at the American Association for Cancer Research (AACR) special conference Hematologic Malignancies: Translating Discoveries to Novel Therapies, held Sept. 20-23.
"Our goal is to identify vulnerabilities in cancer across stages of tumor evolution while it is developing resistance to initial treatment, to help guide the design of drug combination strategies," said Douglas Lauffenburger, PhD, professor in the Department of Biological Engineering and Koch Institute for Integrative Cancer Research at MIT in Boston.
"There may be many stages in a tumor evolution while under treatment that may make them vulnerable to already existing therapies," Lauffenburger continued. "Rather than waiting for the tumor to become resistant to the first treatment and then thinking about a second-line drug to use, we can capitalize on opportunities that exploit vulnerabilities at different early stages, as the tumor is evolving to become resistant to the first drug."
In an initial screening experiment using a combination of computational and experimental approaches, Lauffenburger and colleagues Boyang Zhao and Michael Hemann identified drugs that are likely to be effective against a murine acute lymphoblastic leukemia (ALL) cell line as the cells evolve. These drugs were effective against certain human chronic myelogenous leukemia (CML) cell lines as well.
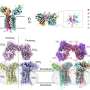
Next, to develop drug combinations based on the characteristics of evolving tumors, the researchers used escalating doses of the drugs imatinib, dasatinib, nilotinib, foretinib, and crizotinib on ALL cells. As some cells exhibited resistance to a particular drug, the research team treated the resistant cells with other drugs to check for cross-resistance. They found that resistant cells surviving at low multiples of the original drug dose actually demonstrated sensitization to certain other drugs, with the sensitization abrogated at higher doses.
"Instead of only looking for the most resistant population of ALL cells at the end of this selection process, we monitored for drug sensitivity of the cells at each stage of the dose escalation," explained Lauffenburger. "This led us to discover the vulnerabilities of a tumor at different stages of clonal evolution, a phenomenon we would have missed if we only analyzed for drug sensitivity at the last stage of this process, which is equivalent to when a patient has relapsed.
"From our studies, we found that, for example, it would be ideal to treat an ALL patient with dasatinib followed by crizotinib/foretinib for synergy during the early stages of clonal evolution of the patient's tumor, rather than treating only with dasatinib and waiting until the patient has relapsed," said Lauffenburger.